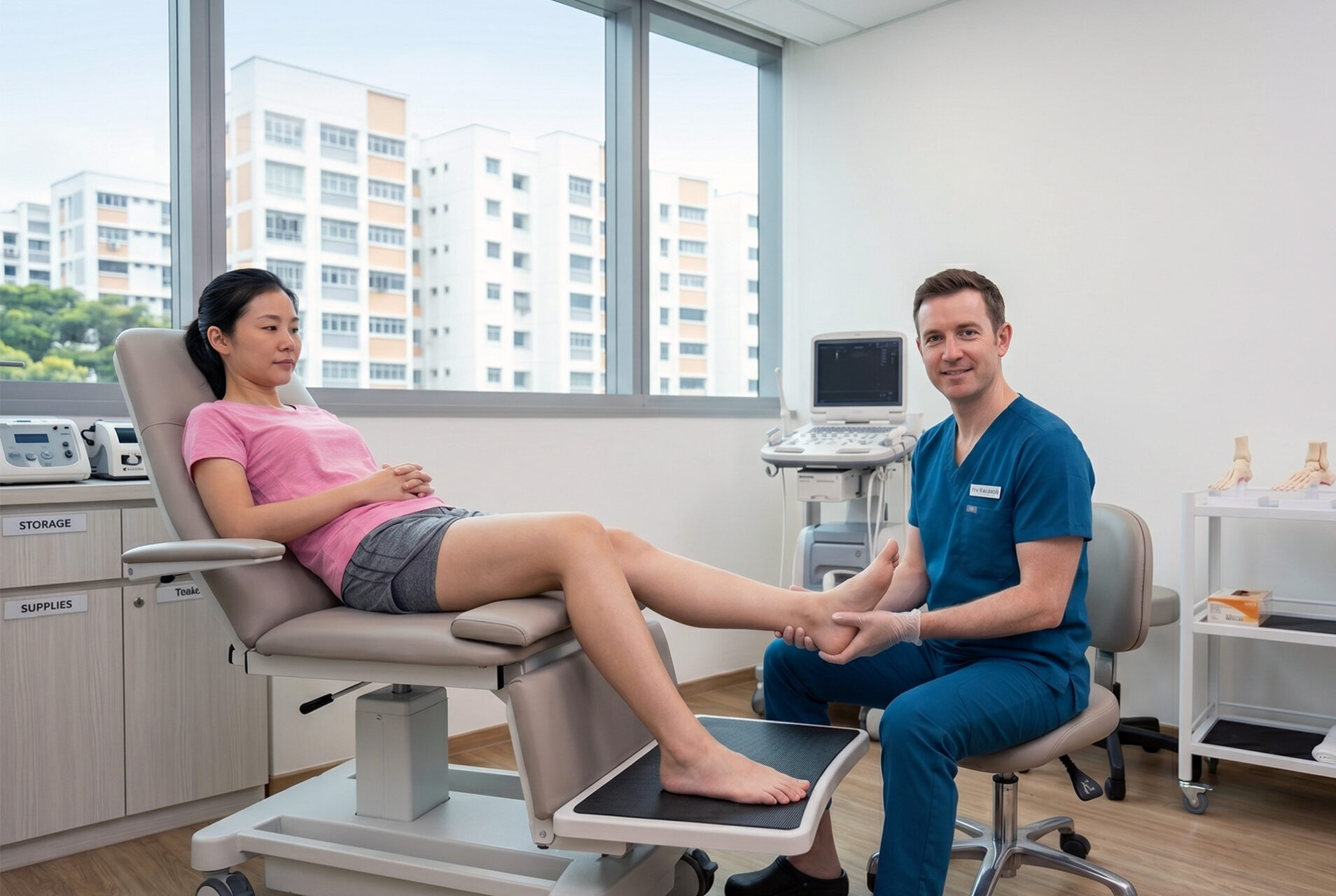
What Is Achilles Tendinopathy?
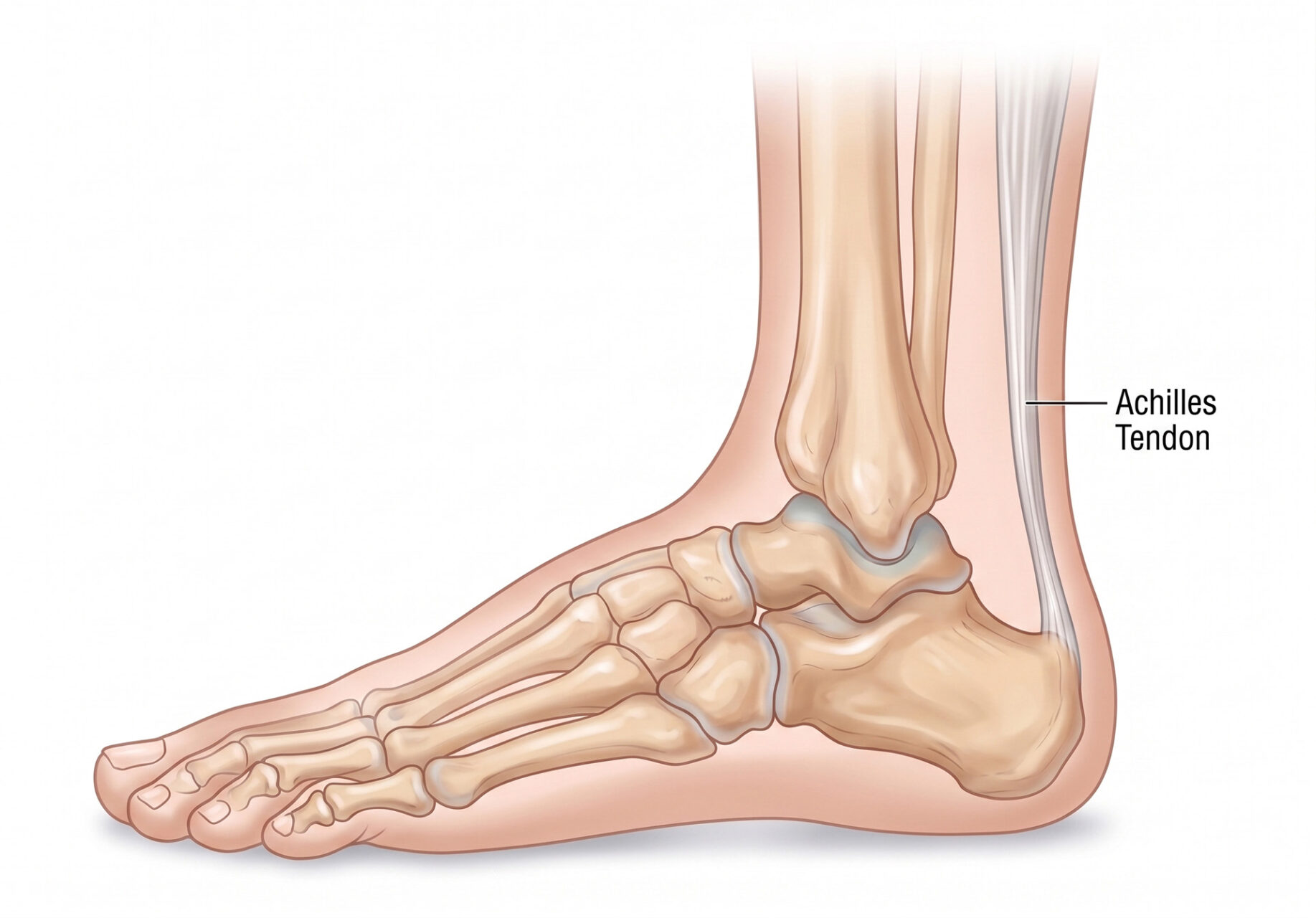
The strongest tendon in the lower leg is the Achilles tendon. This tendon connects the calf muscles to the heel bone and helps you push off when walking, climb stairs, run and rise onto your toes. When this connective tissue becomes irritated and structurally overloaded, Achilles tendon pain, heel and ankle pain, and stiffness can follow. In many, the affected tendon shows a mix of irritation, thickening and changes in the tendon fibres caused by repetitive stress.
Achilles tendinopathy can affect the mid-portion of the Achilles tendon, known as non-insertional Achilles tendinopathy or mid-portion Achilles tendinopathy, usually a few centimetres above the heel bone; or insertional Achilles tendinopathy, where the tendon attaches to the heel bone.
Although Achilles tendonitis and runners are often synonymous, Achilles tendon disorders are not limited to runners. They can also affect tennis players, football players, dancers, active adults who play sports on weekends, and people who dramatically increase their walking. In Singapore, it is common for runners to incur a tendon injury while building towards the Standard Chartered Singapore Marathon, especially when mileage rises faster than the Achilles tendon can adapt.
Achilles Tendinopathy Symptoms
Achilles tendinopathy symptoms usually include Achilles tendon pain, stiffness and tenderness at the back of the heel bone or along the tendon. Symptoms often begin as a mild ache after activity, particularly after a longer run, a hard court session, repeated stair climbing, or hill work. The first few steps out of bed may feel tight and sore, and the calf muscles and tendons may only loosen once you move around. You may experience ankle pain when walking uphill, squatting, sprinting, or pushing up onto your toes.
As the problem worsens, the tendon may feel thickened, warm or slightly swollen. Some may notice a tender lump in the Achilles tendon. Insertional Achilles tendinopathy can feel especially sore when the back of the heel bone is compressed by a stiff shoe counter.
Chronic Achilles tendinopathy can be more limiting. Severe pain may begin earlier in activity, last longer afterwards, and affect everyday walking. These symptoms should not be ignored. The tendon can weaken over time, increasing the risk of a partial tear or Achilles tendon rupture.
Achilles Tendinopathy vs Tendinitis
Achilles tendinopathy is a broader, often chronic term encompassing structural degeneration and microtears in the tendon’s collagen, typically characterised by tendon pain, stiffness, and thickening without significant inflammation.
Achilles tendinitis, also spelt Achilles tendonitis, is an acute, painful inflammation of the Achilles tendon, typically characterised by pain, swelling, and a recent injury, often due to trauma or sudden overuse.
How Achilles Tendinopathy Is Diagnosed
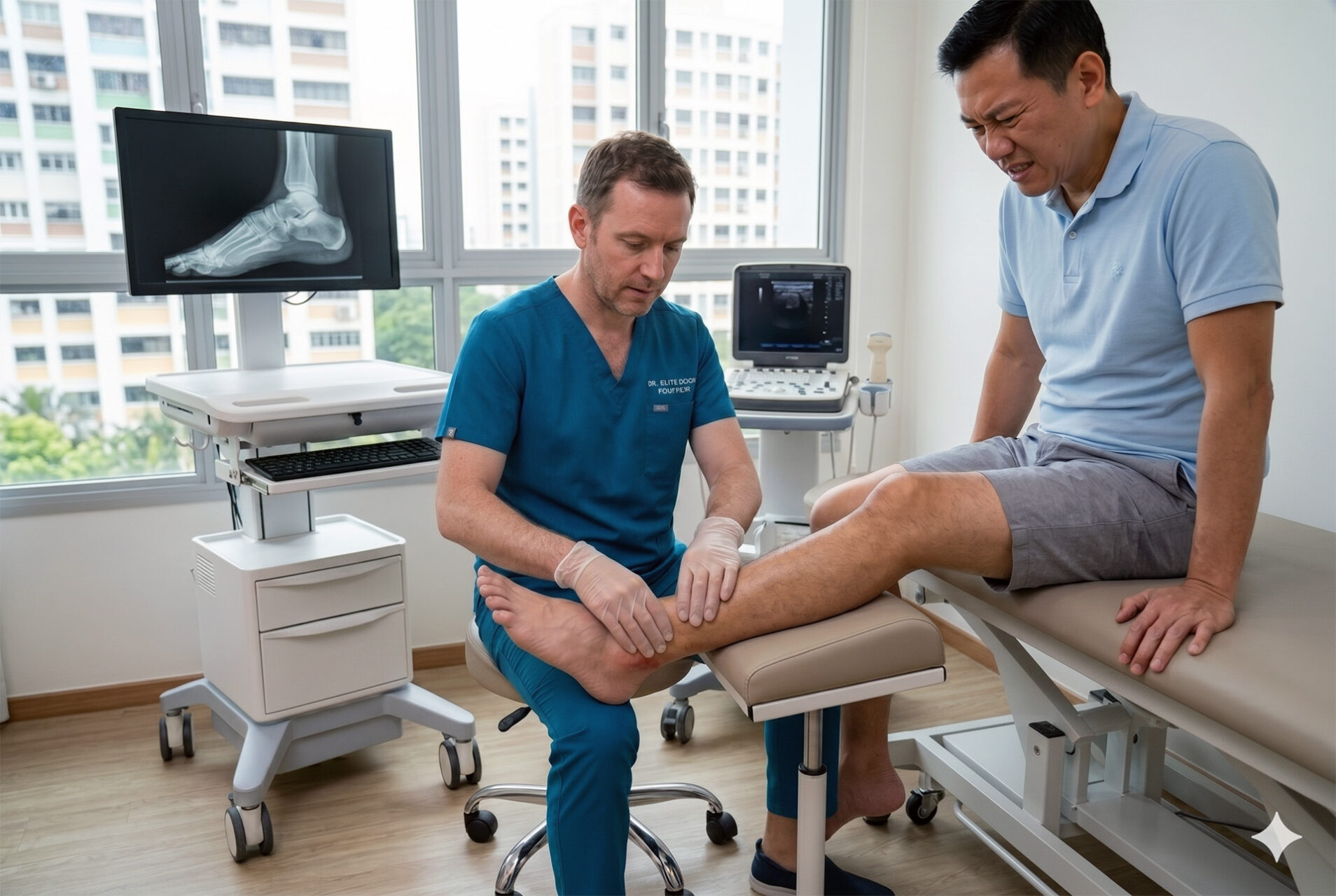
Tendinopathy of the Achilles is diagnosed through a careful history, physical examination and, when needed, imaging to rule out other causes of Achilles tendon pain. Your podiatrist will ask about your training load, footwear, surfaces, occupation, medical history and how the pain behaves during and after activity. This helps distinguish tendon pain from retrocalcaneal bursitis, plantar heel pain, psoriatic arthritis, ankylosing spondylitis, or a tendon tear, all of which demand different management strategies.
At The Foot Practice, diagnosis goes beyond simply pressing the painful Achilles tendon. A podiatrist will assess the tendon for tenderness, thickening, and stiffness, and will examine your calf muscle strength, ankle mobility, single-leg heel raise capacity, and foot loading during walking or running.
RehaWalk® Gait Analysis can be particularly useful when biomechanical factors contribute to Achilles tendon overload. It identifies patterns such as overpronation and asymmetrical loading that may keep the tendon under strain.
Imaging is not always necessary, but it may be recommended if the diagnosis is uncertain, symptoms are severe, or an Achilles tendon rupture is suspected. Ultrasound and magnetic resonance imaging (MRI) can show the tendon thickening, degeneration or tearing. In selected cases, X-rays or blood tests may also be useful, especially if there is concern about bone spurs, insertional Achilles compression, or an inflammatory condition.

When to See a Podiatrist
There is no instant cure for Achilles tendinopathy, but most patients improve with the right podiatric plan.
You should see a podiatrist if Achilles tendinopathy symptoms persist, keep returning, or begin to limit your walking, exercise, or daily activities. Mild Achilles tendon pain after an intense workout may settle with a short period of relative rest. However, tendon pain that lasts more than a few days, flares with activity, or worsens over time warrants a proper assessment.
You should also seek prompt care if the Achilles tendon feels very swollen, if you experience pain with a sudden, sharp popping sensation, or if you struggle to push off the foot, as these features may indicate an Achilles tendon rupture or more serious tendon injuries.
Non-Surgical Achilles Tendinopathy Management
Management usually starts with load reduction, targeted exercises, and correction of factors that overload the Achilles tendon. Proper Achilles tendinopathy treatment matches the severity, location, and the cause of the tendon problem, differentiated into phases of treatment.
- The first step is often relative rest. This means reducing the activities that sharply aggravate the tendon rather than stopping all movement completely. Running, jumping, and hill work should be scaled back for a period and replaced with lower-impact exercise and physical therapy to maintain fitness. Ice can help reduce pain in the more reactive stage. A walking boot may be used in more severe cases to protect the Achilles tendon.
- Achilles tendinopathy exercises and physical therapy are central to recovery. Physical therapy focuses on eccentric exercises and progressive calf muscle strengthening to reduce pain. Depending on the case, physical therapy may include isometric holds for pain relief, eccentric exercises, progressive calf raises, heavy, slow resistance work, calf stretches, and later-stage energy-storage drills such as hopping or return-to-run progressions. Achilles tendinopathy rehab and physical therapy work best when loading is gradual and structured. Too little loading can leave the tendon weak. Too much, too soon, can cause another flare.
- Footwear and biomechanical support are also important. Wear supportive shoes appropriate for the activity. Default to supportive shoes with adequate heel lifts to reduce Achilles tendon strain. RehaWalk® data helps make these footwear recommendations more precise by showing how forces move through the foot and ankle.
- Mobilisation and physical therapy improve movement & flexibility. Mobilisation exercises and physical therapy may be used to improve ankle movement and calf muscle flexibility when stiffness contributes to overload.
- Adjunct therapies may help in selected cases. Dry Needling addresses calf muscle tightness and lower-leg dysfunction. Shockwave Therapy may also be helpful for stubborn or chronic Achilles tendinopathy. Shockwave Therapy is not a stand-alone fix, but can support the broader recovery plan when used appropriately.
Corticosteroid injections and steroid injections into the Achilles tendon itself are generally not a routine first-line option, as steroid injections may increase the risk of tendon rupture and Achilles tendon rupture. Platelet-rich plasma injection may be considered in selected cases as an alternative to steroid injections. That risk is one reason why good diagnosis and progressive physical therapy matter.
Achilles Tendinopathy Surgery
Achilles tendinopathy surgery is usually considered only after a well-structured period of non-surgical podiatric care and physical therapy has failed to manage symptoms, or when there is significant tendon tearing or rupture.
The exact procedure depends on the problem. Surgical treatment may involve removing damaged tendon tissue, repairing split fibres, performing tendon transfer, addressing bone spurs and bony irritation at the heel, or reattaching the Achilles tendon if it is ruptured. Achilles tendinopathy surgery can help carefully selected patients, but it is not a shortcut. It still requires protected healing through physical therapy and structured rehabilitation afterwards.
Risks, Recovery and Achilles Tendinopathy Rehab
Achilles tendinopathy rehab is often gradual because tendons usually recover more slowly than calf muscles. A mild case may improve within weeks, but more established symptoms often take months to resolve. Chronic Achilles tendinopathy usually reflects long-standing overload and tissue changes, so it often requires a longer recovery timeline, physical therapy, and patience.
The main risks of leaving it untreated are recurring Achilles tendon pain, loss of calf muscle strength, muscle power deficits, reduced activity tolerance, and, in some people, tendon rupture.
A safe return to play sports is usually staged. The Achilles tendon should tolerate walking, calf raises, and basic loading without a flare before higher-impact drills are added. People who play sports should reintroduce running volume, speed, and hills one step at a time with guidance from physical therapy. Wear supportive shoes with heel lifts when returning to play sports. If Achilles tendinopathy symptoms return, adjust the plan. Good recovery is not just about pain settling. It is about rebuilding tendon capacity so the Achilles tendon can cope with the demands of life and sport.

How The Foot Practice Can Help
If you have ongoing Achilles tendon pain at the back of the heel bone, morning stiffness, recurring flare-ups or difficulty returning to exercise, The Foot Practice in Singapore can help. For Achilles tendinopathy care, our podiatrists assess not just the Achilles tendon but also your gait, footwear, foot mechanics, and training load to create a personalised management plan.
With the right combination of diagnosis, Achilles tendinopathy exercises, biomechanical support, physical therapy, and staged return to activity, most people can regain function and reduce the risk of recurrence. Contact The Foot Practice today to arrange a sports injury consultation.