Don’t wait until the heel pain becomes debilitating. If the right warning signs are caught early, your plantar fasciitis treatment can help you avoid long-term foot conditions that can present as injuries elsewhere in the body.
Plantar fasciitis (plantar heel pain) is a musculoskeletal disorder affecting the fascial insertion into the heel bone.
Plantar fasciitis is thought to have a biomechanical origin and is associated with higher body mass index and lower-limb biomechanical anomalies. Heel pain is a common ailment, and anti-inflammatory drugs will not help the condition heal.
Plantar fasciitis is a condition that is currently not well understood. However, it is more common in runners and those who are overweight. Did you know that ‘itis’ in clinical terms means ‘inflammation’ of the plantar fascia? It may be incorrect to use the term if the condition is due to tissue breakdown (plantar fasciosis) rather than inflammation. Plantar fasciopathy would be the correct overarching term for the condition, but it is little used.
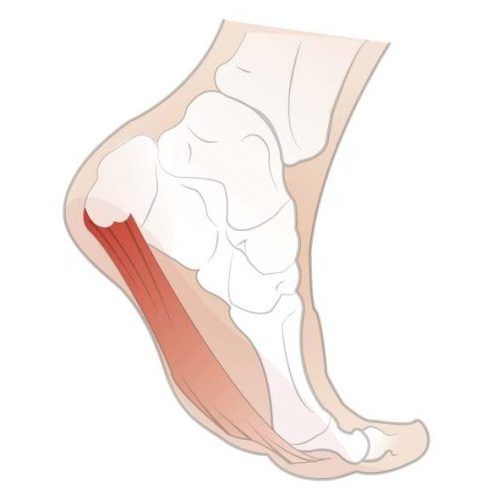
Other injuries are often misdiagnosed as plantar fasciitis, such as heel pad atrophy and pain due to neural origins, calcaneal fractures and other soft tissue injuries. Seeking advice from a qualified healthcare practitioner, like a podiatrist or foot doctor, can help you with the right diagnosis to get the right treatment needed for pain-free movement.
You don’t have to live with heel pain. The most important aspect of treatment is to seek a professional assessment from a podiatrist as soon as possible, before the condition worsens.
To prevent plantar heel pain, your podiatrist may provide you with the following:
- Assist you with taping, using adhesive tape to provide the foot with more support.
- Design prescription or custom-made insoles for plantar fasciitis.
- Teach you stretches for plantar fasciitis and for your calf muscles to relieve pain.
- Advise you on both your running shoes and non-athletic daily footwear. Inadequate support, whether with high heels or an uneven distribution of weight across the sole, can exacerbate plantar pain.
- Provide Shockwave Therapy for plantar fasciitis to help alleviate heel pain in patients who have been unaffected by conventional treatments.
- Assess your body to see if your weight or posture is compounding the issue.
How to Alleviate Pain from Plantar Fasciitis: Effects and Treatment
During walking, running, and standing, the plantar fascia acts as a cushion and stabiliser, bracing the arch of the foot. However, when there is too much pressure on the plantar ligament, such as when carrying more body weight, when the pressure increases suddenly due to weight gain (e.g. pregnancy), or when the pressure is overly repetitive, as in long-distance running.
Plantar heel pain can make everyday activities like walking difficult and running beyond uncomfortable. In fact, heel pain can be caused by any activity, even cycling, that engages the feet and arches. It can be a frustrating condition to live with, but there are many treatments available.
Diagnosis often relies heavily on clinical signs, such as heel pain after periods of inactivity, like waking up in the morning, or pain that fades throughout the day but increases during exercise.
And if you’re experiencing heel pain when running, read our article about whether footwear plays a role and the top 5 shoe recommendations from our lead podiatrist, Tim Maiden.
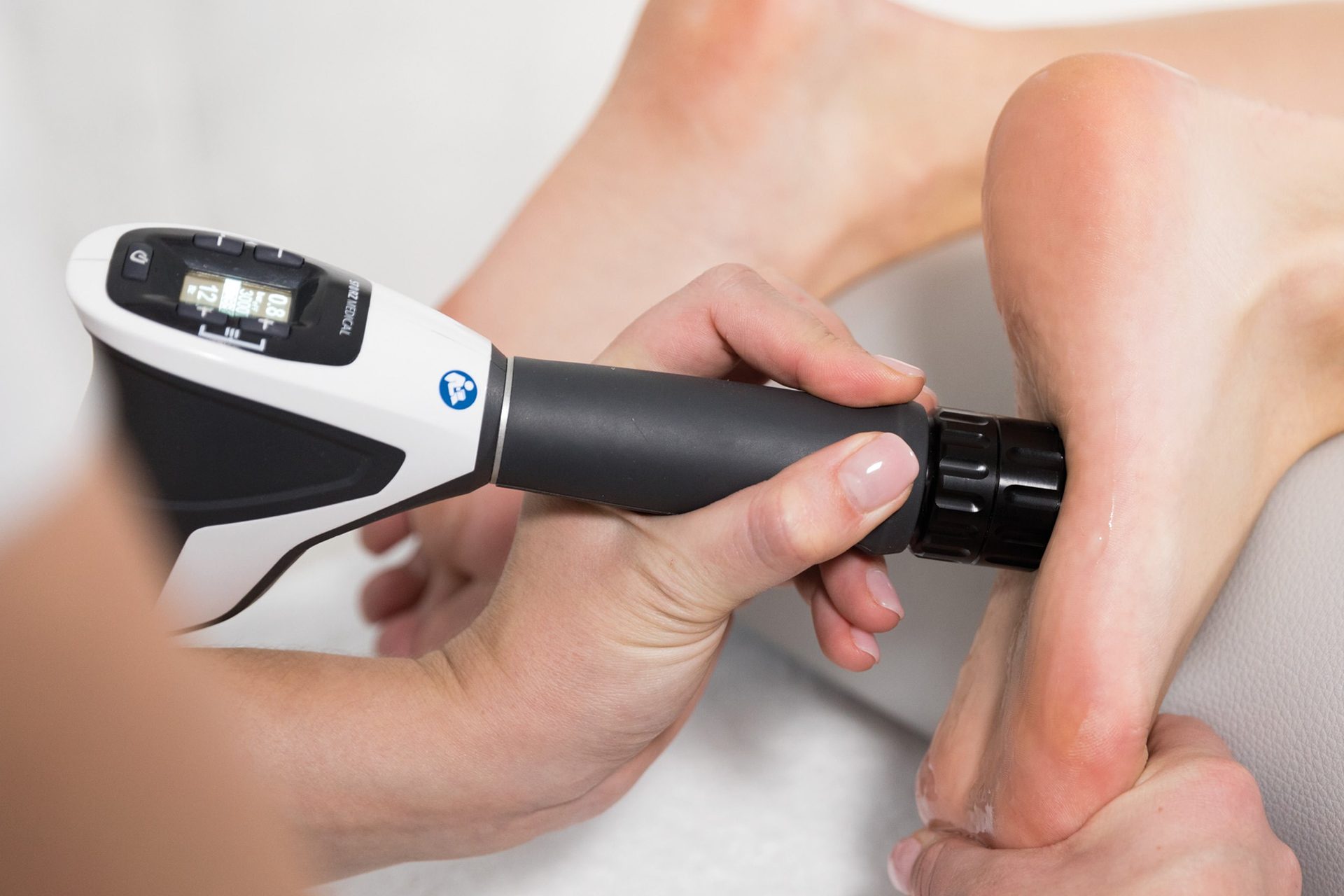
Initial treatments work to reduce pain by limiting activity and standing, in addition to using foot-arch support insoles in the shoes. Anti-inflammatory drugs may also be prescribed to reduce possible inflammation. Fortunately, it has been reported that most patients respond to conservative treatment [1] like orthotic therapy, Shockwave Therapy, foot activation exercise, etc., to help alleviate pain.
Why Big Toe Facilitation Matters to Prevent Plantar Fasciitis
Plantar fasciitis, which can stem from pronation, can result in excessive foot pronation. Pronation of the subtalar joint, near the ankle, everts the calcaneus – the bone within the heel – thereby increasing the intrafascial tension and worsening the initial condition.
The big toe, or hallux, is essential to foot health. The hallux controls the foot’s arch and maintains stability, ensuring that impact is distributed evenly across the foot with each step.
Your hips and legs connect to the ground through your feet, so each step’s impact affects the efficiency of your gait. If your hallux isn’t working as it’s meant to, that impact can get sent through your leg the wrong way, affecting tissues not accustomed to those forces. Over time, those repeated traumas lead to injury.
To go deeper into why the hallux matters for your gait, it’s worth understanding the mechanism with which it assists the leg in stepping. That mechanism is called the windlass mechanism, where the hallux pulls on the plantar fascia of the foot, creating tension. This tension raises the arch, stiffens the foot and enables a strong push-off. The stiffness makes the foot a rigid lever, while the plantar fascia pushes against the ground, making for a healthy step. [2]
One cause of plantar fasciitis is prolonged pronation or flattening of the foot arch, which increases strain on muscles and ligaments. People with pronation problems have a more flexible, lower-arched foot. Effective treatment depends on controlling pronation. Excessive pronation can be caused by muscle weakness, tight Achilles tendons, and abnormal foot structures.
Stretches for Plantar Fasciitis Injury
The key message for patients with this condition should be that they must perform exercises, or their symptoms will reappear. These can include high-load strength training.
High-load strength training may help to reduce pain and improve function more quickly. A simple progressive protocol performed every other day results in better self-reported outcomes than plantar fascia-specific stretching. A couple of plantar fascia stretches may include:
- Pulling back the big toe and massaging the foot arch
- Heel raises with the toes elevated under a towel
Remember that before you begin any exercise or stretching, we highly recommend making an appointment with a specialised healthcare provider to properly diagnose your condition. Self-diagnosing and treatment can lead to further complications and injuries down the road.
Where to Buy Orthotic Insoles for Plantar Fasciitis in Singapore
One common treatment for plantar fasciitis is the use of plantar fasciitis orthotics to address imbalances in walking gait or foot strike. Orthopaedic insoles for plantar fasciitis can help with your pain and prevent your condition from getting worse. Custom orthotic insoles raise the medial longitudinal arch of the foot, immediately relieving pain by reducing tissue stress during standing and ambulation.

In addition to orthotic therapy, stretching exercises to activate the big toe are effective for reducing inflammation and relieving discomfort associated with plantar fasciitis.
If you’re wondering if over-the-counter or custom-made insoles are the best for plantar fasciitis, read our article about the benefits of prescribed insoles versus store-bought. One of the best arch support insoles for plantar fasciitis in Singapore is The Foot Practice’s carbon fibre insoles by Footworks podiatric laboratory.
Plantar fasciitis is a cause of chronic heel and bottom-of-foot pain and is one of many conditions that affect the foot. It’s important to address plantar fasciitis as it arises, as studies suggest that if left unattended, it can lead to a vicious cycle. When your foot is affected, your daily activities and your exercise routines can be significantly hampered.
Stretching, in conjunction with custom-made orthotics for plantar fasciitis from The Foot Practice, can bring you on the path to recovery. Make your appointment with The Foot Practice sports podiatrist today so we can figure out the best way to support your foot, whether that’s custom insoles, stretching exercises, or other healing methods.
Related Plantar Fasciitis
———-
Sources
[1] Yu H., Randhawa K., Côté P., Optima C. The effectiveness of physical agents for lower-limb soft tissue injuries: a systematic review. Journal of Orthopaedic and Sports Physical Therapy. 2016;46(7):523–554. doi: 10.2519/jospt.2016.6521
[2] Bolgla LA, Malone TR. Plantar fasciitis and the windlass mechanism: a biomechanical link to clinical practice. J Athl Train. 2004;39(1):77-82.






