What Is IT Band Syndrome?
The iliotibial band (ITB) plays a key role in stabilising the knee and storing and releasing energy during running. It is a thick band of connective tissue that begins at the pelvic bone and runs along the outside of the thigh and thigh bone to the lateral epicondyle (the bony prominence) of the knee joint.
IT band syndrome (ITBS), also known as ‘runner’s knee’, is a common overuse injury that causes sharp pain on the outside of the knee in runners. It is usually a load-related issue when the body cannot adapt fast enough to the increasing load. Most runners improve with a clear plan that reduces irritation, builds hip and leg strength, and helps them return to running in gradual steps.
For years, IT band syndrome was described as repetitive friction, with the IT band ‘rubbing’ over the lateral femoral epicondyle of the knee. However, current sports medicine thinking more often describes a compression problem, in which repeated knee bending under load compresses the tissues beneath the IT band. This shift is important because treatment and physical therapy now focus on progressive loading rather than simply on releasing tension in the IT band.

Why Do Runners Get IT Band Syndrome?
IT band syndrome is common among novice runners and among runners returning from a break who ramp up quickly. It is also common among trail runners and long-distance runners, where downhills and narrow singletrack increase side-to-side knee demands. Training errors, such as excessive running volume or sudden changes in training, are frequent triggers of IT band syndrome.
Runners often develop IT band syndrome when the training load and terrain demand more lateral knee control than they are prepared for. In simple terms, the iliotibial band helps manage lateral loads on the leg. Downhill running, running on cambered roads, fatigue late in a run, and sudden volume increases can all increase compressive stress on the outside of the knee. A crossover gait pattern, in which one leg crosses in front of the other in the same direction, can also increase IT band tension.
Who Is Most Likely to Develop IT Band Syndrome?
IT band syndrome is among the more common running injuries and often follows a training spike rather than a single incident. Prospective research has also shifted old assumptions. IT band syndrome isn’t something exclusive to female runners, nor is it an issue of compression alone.
You may be more likely to develop symptoms if you have one or more of these patterns if you:
- Are a new runner, building distance quickly
- Are you returning after time off
- Run trails or do frequent downhills
- Run long sessions on cambered routes
- Add speedwork, hills, or intensity too quickly
If you are very experienced and develop new outer knee pain, be cautious. Other conditions can mimic IT band syndrome, including bone stress injuries around the thigh bone, which require a different treatment plan. A correct diagnosis from a healthcare provider, such as a podiatrist, makes all the difference.
Symptoms of IT Band Syndrome
IT band syndrome symptoms typically involve localised pain on the outside of the knee that begins during a run, often at a consistent time or distance. It is common to notice IT band pain after running, with soreness that lingers into the next day. You may experience more pain in one leg than in both, depending on your running style and the terrain.
Common symptoms include:
- Pain on the outside of the knee during running, especially running downhill
- Pain that eases with rest and returns when you run again on the outside of your knee, sometimes slightly above the joint line
- Discomfort walking downstairs during a flare-up, particularly when placing one leg forward and slowly lowering your weight onto the other leg
- A flare-up on the day after a provoking session
Your podiatrist may perform a physical examination, including the Noble compression test or Ober’s test, to help confirm IT band syndrome. Seek assessment sooner if your pain is severe at rest, present at night, associated with swelling, or very focal to the bone, as these features may indicate a diagnosis other than IT band syndrome.
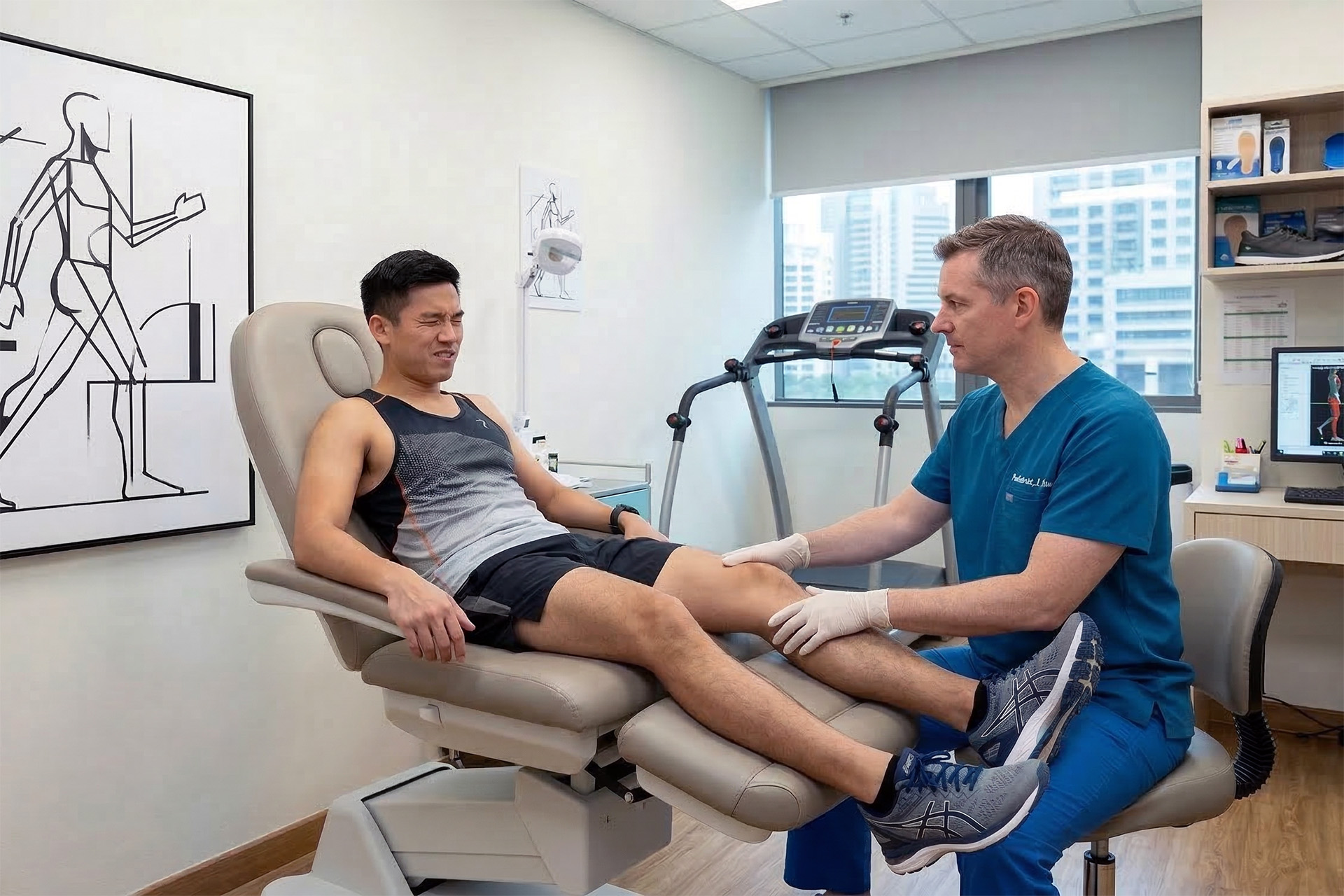
What Causes IT Band Syndrome?
IT band syndrome is typically caused by training errors combined with running demands that increase lateral knee compression before the body has had time to adapt. You do not need a ‘tight IT band’ for this to happen. The iliotibial band is meant to be firm. It is part of the body’s natural energy storage and release.
Common triggers include:
- A sudden jump in weekly mileage or long run distance
- Introducing downhills, trails or speedwork too quickly
- Running on a single track with a narrow step width
- Running on roads with a strong camber
- Fatigue and reduced hip control late in runs are often linked to hip abductor weakness or weak hip muscles
Biomechanics can matter, but not always in the way people expect. Overpronation is often blamed, but a more useful pattern to assess ITBS is overstriding, in which steps are long and the leg swings forward, causing the foot to land too far in front. This can alter braking forces and the lateral load on the knee. An excessive hip drop can also increase the IT band compression and impose excessive strain on the thigh.
If you have a sore IT band from running, the cause is often the combination of a recent training change and the type of running you are doing, rather than a single structural fault. A thorough diagnosis by a healthcare professional helps rule out other causes of pain outside of your knee.

When To See a Podiatrist
Consider an assessment by a podiatrist if your symptoms prevent you from running, recur, or do not improve after two to three weeks of load changes. It is also worth assessing whether the pain is worsening, present at rest, or inconsistent with typical IT band patterns. A good assessment confirms the correct diagnosis and identifies the smallest set of changes that will make all the difference in your long-term recovery from this condition. IT band syndrome can be frustrating, but it is not a mystery when you consider load, movement, and capacity together.
Can You Run Through IT Band Pain?
If you are tempted to run through IT band pain, know this: if pain increases quickly, changes your running form, or worsens that day or the next, pushing through often prolongs the problem. The required rest depends on the severity. If symptoms are mild and settle quickly without a next-day flare-up, a carefully modified run may be reasonable, but it should be part of a careful and deliberate plan, not an impromptu test.
Management of IT Band Syndrome for Runners
IT Band Syndrome Treatment: What to Do First
The first step is to reduce irritation while keeping you active without provoking symptoms. Complete rest often leads to loss of capacity, then relapse when you return to running.
Start with these priorities:
- Reduce the main trigger for a short window, such as downhills, speedwork, or long continuous runs.
- Choose lower-irritation cross-training, such as cycling, brisk walking on level ground, or treadmill walking at an incline, to maintain fitness.
- Avoid repeated test runs that only lead to flare-up symptoms every few days.
- Watch the next day’s response, not only how you feel during the run
Uphill treadmill walking is a practical option because it reduces the impact of downhill running. Some runners also naturally widen their base of support when walking uphill, which can reduce lateral knee stress.
Why You Should Reconsider Foam Rolling for IT Band Syndrome
Stretching and aggressive foam rolling of the IT band are often ineffective because they can increase compression in an already irritable area, making any relief short-lived. Applying a foam roller directly to the IT band can exacerbate symptoms. Some runners feel temporarily better because strong pressure can briefly desensitise the nervous system. However, this does not build capacity.
Instead, foam rolling the surrounding muscles, such as the hip flexors, quadriceps and calves, may provide greater benefit without compressing the irritable IT band. Gentle foam rolling of these areas, combined with hip movement drills, can complement a strengthening programme, but is not enough to treat IT band issues alone.
A more durable plan focuses on calming the symptoms first, then rebuilding strength and resilience so you can tolerate the running that triggered the pain.

IT Band Syndrome Physical Therapy
Physical therapy exercises help patients build hip and leg control and knee stability before progressing to heavier loading and running-specific drills. Early work often includes hip abductor and hip flexor strengthening exercises, along with controlled range-of-motion exercises to maintain knee comfort. Hip-strengthening exercises, particularly for the hip abductors and hip adductor control, play a key role in long-term recovery from IT band syndrome.
A practical progression often looks like this:
- Early stage: Reduce provocation, maintain fitness with cross-training, and begin strengthening exercises and stability work. Manual therapy to the hip flexors and surrounding muscles may help relieve stiffness.
- Middle stage: Build heavier strength work, often using split-squat variations and a progressive load. Focus on hip adduction control and single-leg exercises, such as standing on one leg and slowly lowering into a squat. Manual therapy may continue alongside progressive loading.
- Late stage: Add plyometrics and running drills to restore energy storage and release capacity. Practise drills that involve driving the leg forward to build running-specific power. Upper-body and hip movement exercises can also help restore full coordination.
IT band syndrome rehabilitation should be guided by your podiatrist and tailored to your running goals. The goal is not to collect a wide range of exercises. The goal is to build load tolerance so that running does not trigger pain. If you are seeking IT band exercises for strength and running training, consider them in these progressive stages after discussing them with a podiatrist.
Gait Retraining
Running gait retraining can help, but it is often best used as a short-term bridge rather than a permanent overhaul. The aim is to reduce the load on the IT band while strength and capacity catch up. One simple cue to assist is a small increase in cadence, which often shortens stride length and reduces overstriding. It can also influence step width without you having to focus on running wider, which some runners find awkward. Adjusting your running style and running shoes may also reduce load on the outer knee.
As symptoms subside and capacity improves, runners can drift back toward their natural running style, provided training load is increased gradually. Most runners can return to pain-free running within a few weeks to a few months with the right approach.
Returning to Running Without the Relapse Loop
A safe return to running is guided by symptoms during the run and by the response the next day. Some runners feel well during the mid-run period, then experience symptoms soon after. That indicates the tissue is not yet ready for that load. A common progression is to start with shorter, flatter runs, build frequency before distance, and add downhills and speed last. For runners recovering from this overuse injury, the goal is to return to running pain-free, so they can train without a predictable flare. Running with IT band syndrome is possible when symptoms are well-managed. However, running through IT band pain without a plan often leads to setbacks.

How The Foot Practice Supports Runners with IT Band Syndrome
Sports podiatry plays a critical role in treating ITBS by addressing biomechanical causes originating in the feet. At The Foot Practice, we support runners in Singapore by combining clinical assessment with data-informed insights and practical progression.
- Footwear assessments: Footwear can affect stability, stride mechanics, and force transmission up the kinetic chain. We assess shoe fit, support, wear patterns, and whether a recent shoe change may have altered leg load distribution.
- RehaWalk® gait analysis: RehaWalk helps us visualise how pressure is distributed through your feet during walking and running. IT band syndrome is felt at the knee, but foot loading can influence leg rotation and knee control during stance. Pressure data can also help track progress over time.
- 3D running gait analysis: 3D infrared gait analysis provides objective insight into cadence, stride length, symmetry, and hip movement patterns that may raise lateral knee load. This can be useful for identifying excessive hip drop, crossover gait, overstriding, and other changes that may occur under fatigue.
- Custom orthoses, when appropriate: Orthoses are not a default intervention strategy for IT band issues, but they can help selected runners, especially if their foot mechanics contribute to inconsistent loading or when shoe stability varies from run to run. The aim is to support efficient, repeatable loading, not to fix pronation.
- Strength progression and mobility work: A structured plan for hip- and leg-strengthening is central to the approach. We guide progression from early stability work to heavier loading, then return-to-run planning, to reduce stop-start relapses.
This approach also accounts for local running conditions, such as long, humid sessions along East Coast Park and trail runs with repeated downhills. IT band running issues improve when you connect symptoms to how you move, what you wear, and how you train, rather than chasing a single tight structure. Contact The Foot Practice today.






