What Is Retrocalcaneal Bursitis?
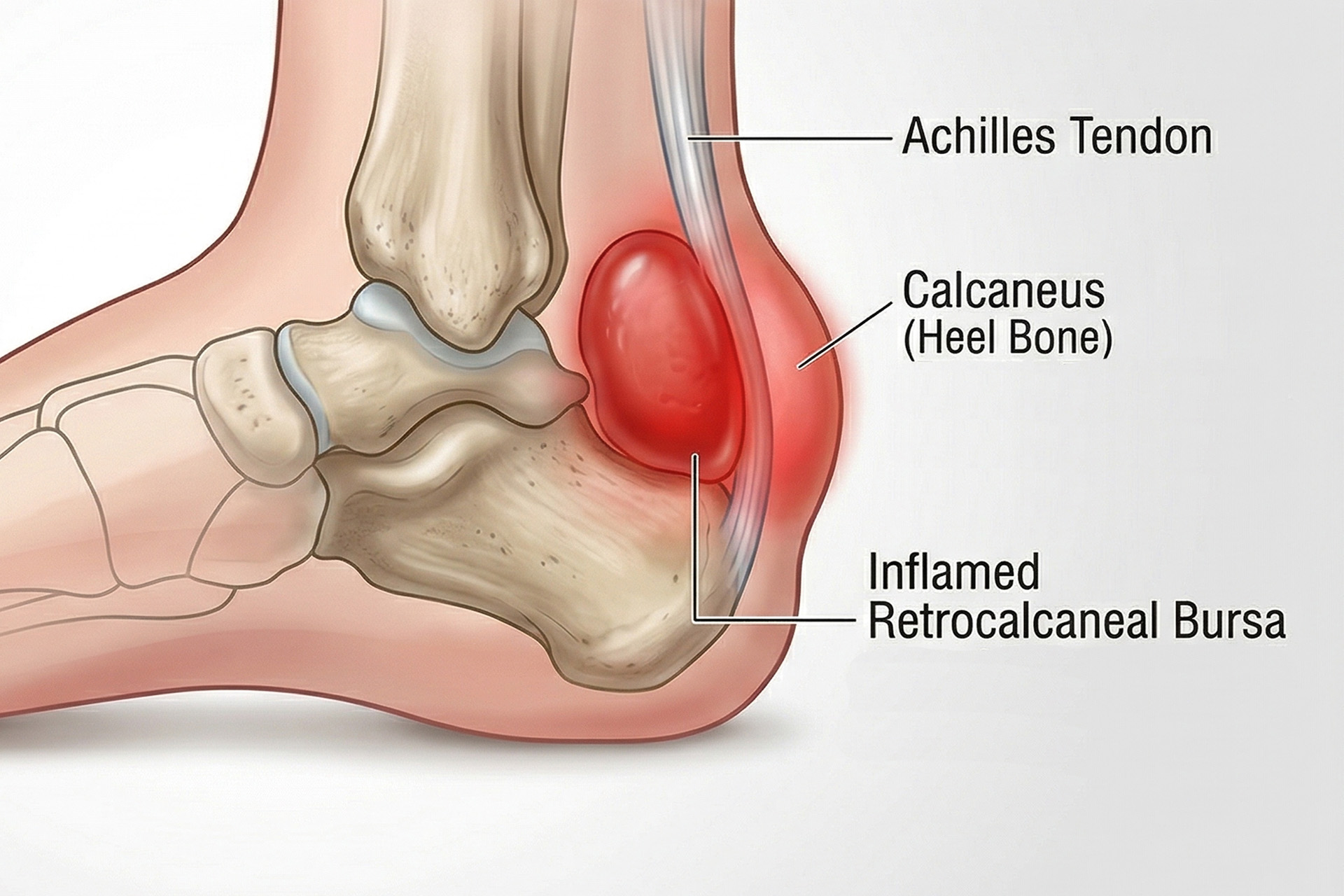
Retrocalcaneal bursitis is a common source of heel pain in the adult foot. It happens when a small, fluid-filled sac – the retrocalcaneal bursa – at the back of your heel becomes irritated and swollen.
The retrocalcaneal bursa acts as a natural cushion filled with synovial fluid. It plays a significant role in reducing friction between the Achilles tendon and the posterior heel during movement, preventing tendon damage. If that area is squeezed or rubbed excessively due to mechanical irritation, the affected bursa can become inflamed and swollen, causing pain, local swelling and heel bursitis.
Retrocalcaneal bursitis, also known as Achilles tendon bursitis, is common among runners, particularly after extensive hill training or a rapid increase in mileage. It can also affect recreational athletes, dancers, and anyone who spends long hours in stiff or tight-fitting shoes. Because the signs of this condition can be very similar to Achilles tendon pain, Achilles tendinitis, or Achilles tendinopathy, it is important to obtain an early, careful evaluation to ensure you reach the correct differential diagnosis.
What Causes Retrocalcaneal Bursitis?
Retrocalcaneal bursitis is commonly caused by the overuse and excessive loading of the ankle. In runners, the most common trigger of retrocalcaneal bursitis is increasing training volume or intensity too quickly without sufficient recovery. Poorly fitting shoes with a rigid heel counter can produce excessive pressure and exacerbate symptoms.
Poor body mechanics and biomechanical abnormalities are frequently a contributing factor. For example, tight calf muscles can restrict dorsiflexion, thereby intensifying the compression at the junction of the Achilles tendon and the heel, particularly during the push-off phase of walking or running. Foot structure, whether a high arch or an excessive pronation, can also affect the distribution of forces across the foot. Furthermore, an abrupt change in footwear, such as switching from high-heeled shoes to flat shoes, can trigger symptoms because the Achilles and bursa must adjust to a new resting length and position.
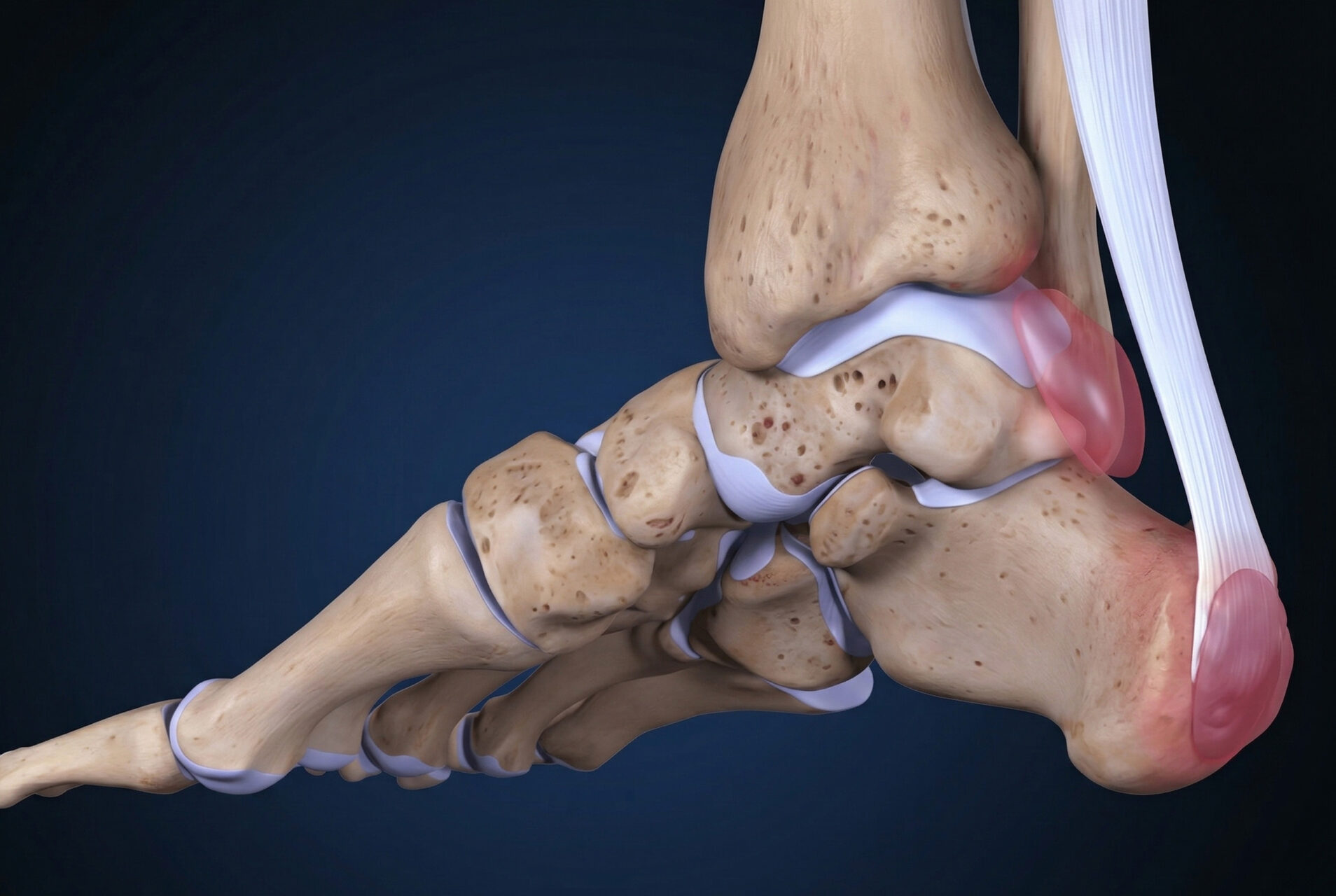
Haglund’s syndrome, Haglund deformity, and retrocalcaneal bursitis are closely linked, and chronic inflammation can develop if the impingement is not addressed. Retrocalcaneal bursitis Haglund’s deformity occurs when an excessively prominent posterosuperior aspect of the calcaneus reduces the space for the retrocalcaneal bursa. It is most pronounced during uphill walking, running and stair climbing.
Less commonly, inflammatory conditions such as rheumatoid arthritis or gout can also inflame the bursa, as can a direct blow to the back of the heel. In severe cases, the subcutaneous calcaneal bursa (a separate subcutaneous bursa located behind the Achilles) and the subtendinous bursa may also become involved.

Symptoms
Retrocalcaneal bursitis symptoms often develop gradually. The main sign of this condition is heel pain at the back of the foot, right where the Achilles tendon inserts, that feels deep and throbbing. It can worsen when you push off the ground while walking or running, when you ascend stairs, when you stand on your toes, or when you wear shoes that rub or press on that area.
Many patients notice a pattern in which discomfort worsens at the start of activity, improves as the body warms up, and then recurs later after the body has cooled down. That pattern can lead them to push through early symptoms, thereby prolonging inflammation. Over time, you may see local swelling or a soft, warm fullness on either side of the tendon near the heel. If the tenderness is most severe when you squeeze the sides of the lower Achilles insertion site, the bursa is more likely the primary driver than the tendon itself.
If you have redness, increasing warmth, fever, or feel unwell, seek prompt medical evaluation. Infection is uncommon but requires urgent care when present.
Diagnosis
Diagnosis begins with a focused history and a hands-on physical examination. Our podiatrist trained in sports medicine at The Foot Practice will assess where tenderness is most intense: bursal inflammation is often deepest at the sides of the tendon insertion, whereas Achilles tendinitis or discomfort is usually felt along the tendon itself.
Range-of-motion testing and gait assessment of the ankle and foot will help identify factors such as limited dorsiflexion, calf tightness, or loading patterns that may be repeatedly compressing the bursa.
A physical examination is often enough. If symptoms persist, are unclear, or Haglund’s syndrome is suspected, imaging can help confirm the diagnosis or identify bony changes.
Ultrasounds can show fluid in the bursa and assess the Achilles tendon in real time. A weight-bearing lateral X-ray may reveal a bony prominence at the calcaneus or lateral expansions of the retrocalcaneal recess. Magnetic resonance imaging (MRI) can help distinguish bursal inflammation from insertional Achilles tendinopathy when the differential diagnosis is complex.
Podiatry for Retrocalcaneal Bursitis Treatment
Podiatry is a key component of effective treatment for retrocalcaneal bursitis. It helps ease your symptoms and addresses the mechanical issues that keep irritating the bursa.
At The Foot Practice, the RehaWalk® pressure sensor treadmill gait analysis is used to understand how you load through the heel and rearfoot during walking and, if relevant, running.
RehaWalk can highlight patterns such as early heel lift, prolonged loading through one side of the heel, or compensation linked to calf tightness and restricted ankle movement. This information helps guide footwear changes, decide whether a short-term heel lift is likely to help, and tailor a progressive strengthening plan so you can return to your activity safely and securely.

Your podiatrist may suggest:
- Rest: Taking a break from activities that worsen your symptoms.
- Icing: Applying ice for short periods.
- Footwear adjustments: Choosing shoes without stiff heel counters.
- Heel lift: Using a small lift inside your shoe, which can sometimes reduce compression in the short term.
When appropriate, adjunctive modalities may be used to help settle irritability and support progress:
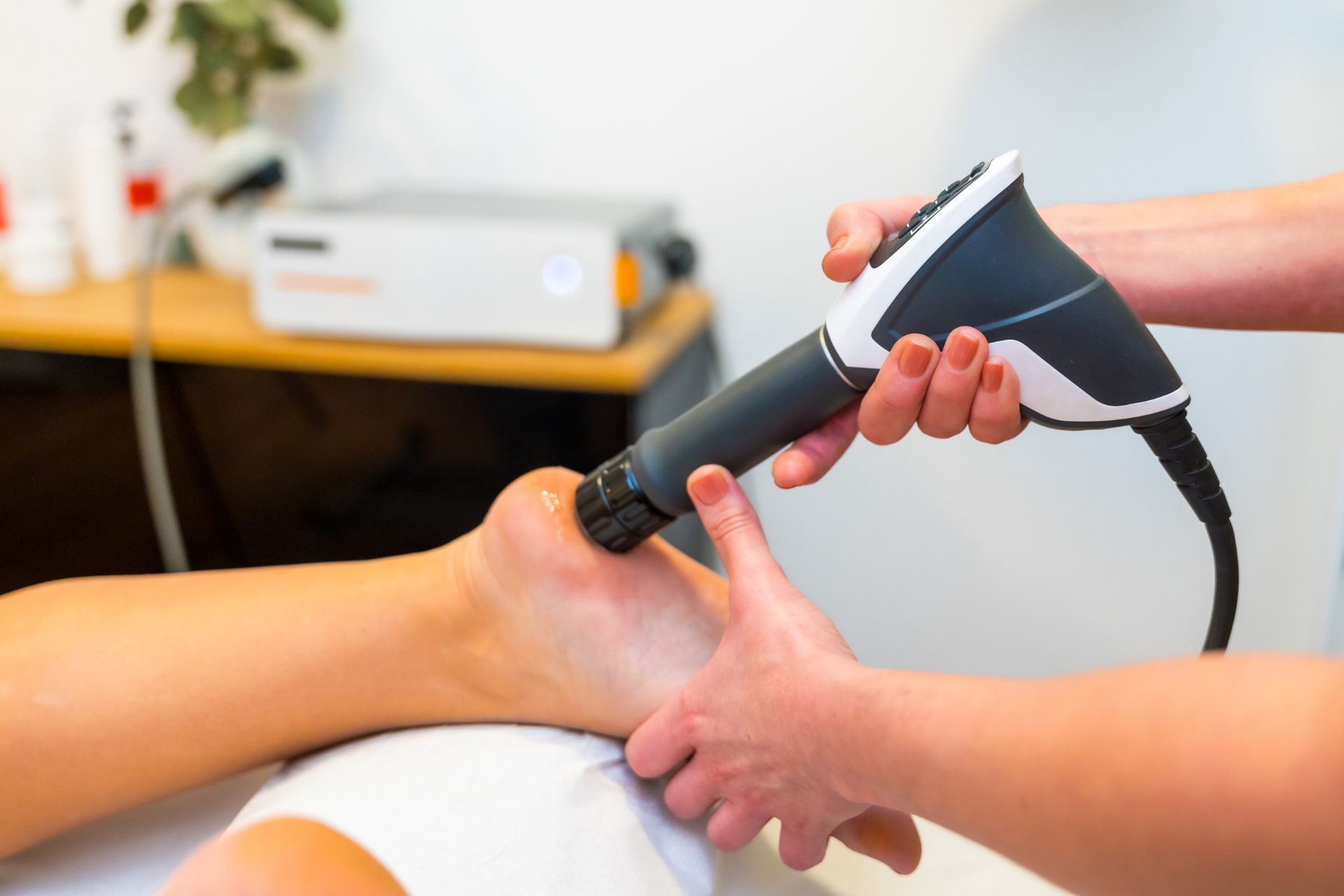
- Shockwave Therapy may be considered. Focused Shockwave Therapy uses energy waves directed at the inflamed area, often at the tendon-bone junction. Radial Shockwave Therapy uses energy waves to relax tight muscles and connective tissue in the calf and around the ankle, potentially reducing sensitivity.
- Dry Needling and manual therapy can help reduce inflammation, ease calf tightness, and address trigger points that restrict motion and increase compression at the back of the heel.
- Orthoses may be considered when foot mechanics and pressure patterns consistently increase compression at the back of the heel. In selected cases, custom orthoses help redistribute forces through the foot, improve rearfoot control, and reduce excessive motion.
As the inflammation settles, rehab will shift towards restoring your mobility and building tissue capacity. Retrocalcaneal bursitis exercises typically begin with calf mobility and strengthening exercises that do not aggressively compress the posterior heel. Strength work will then progress from isometric holds to heavier loads under professional guidance. Some patients do well with heel-lowering strength work, but for some, deep bending can increase compression, so your podiatrist may modify range and technique to protect the bursa while you build strength.
Support strategies can help during your return to activity. Retrocalcaneal bursitis taping may reduce irritation by offloading the area and improving control during walking and training. The goal is a heel that can withstand your usual walking, running, and other sports without recurring flare-ups.
In Singapore, we often see flare-ups after a training spike, such as adding hills around Bukit Timah or increasing court sessions during a busy month. Your plan should account for real life, not just ideal training weeks.
When Surgery Is Considered
Retrocalcaneal bursitis surgery is usually reserved for patients who do not improve after months of consistent conservative care. In severe cases, surgical treatment may involve removing the inflamed bursa. If Haglund’s deformity is present, surgical treatment may also reshape the bony prominence to reduce the ongoing compression of the posterior heel.
The retrocalcaneal bursitis surgery recovery time varies depending on the type of surgery and the extent of the surgical work. Generally, recovery involves avoiding weight on the foot for a few weeks, followed by wearing a walking boot, and then a personalised physical therapy programme. Most patients can resume daily life within a couple of months, though returning to sports may take longer. Proper treatment and surgical treatment planning can make all the difference.
In some cases, an injection may be considered part of medical care, but it must be approached carefully at the Achilles tendon insertion. Your clinician can advise whether it is appropriate for your situation and what precautions are needed.
Preventing Recurrence
To prevent the recurrence of heel bursitis or retrocalcaneal bursitis, you should remember the following:
- Reduce compression and improve heel load tolerance.
- Maintain calf flexibility and foot mobility with regular exercise.
- Gradually increase running volume and intensity, but be cautious with hills and speed work.
- Rotate through footwear, especially if you wear heels or dress shoes
- Avoid rigid heel counters.
More importantly, pay attention to early aches. Early load modification and strengthening are often more effective than pushing through persistent symptoms.

How The Foot Practice Can Help
If discomfort at the back of the heel is limiting your training or daily activities, early assessment by a medical professional can facilitate your recovery. At The Foot Practice, we combine a detailed biomechanical assessment with prescribed exercises and, when appropriate, adjunctive modalities for retrocalcaneal bursitis. Contact us to book an assessment and start on a plan to help you return to activity.