What Are Shin Splints?
Medial tibial stress syndrome, the scientific name for shin splints, is typically caused by excessive, repetitive stress on the muscles, tendons and bone tissue of the lower leg. The shin bone, muscles, tendons and bone absorb force during physical activity, and when that force exceeds capacity, shin splints develop.
Shin splints are a common overuse injury for runners that develop when the shinbone and the tissues attached to it are overloaded faster than the body can adapt.
Shin splints usually manifest as pain along the inner edge of the shin bone, where muscles attach to the bone. This usually happens after a sudden increase in training intensity, duration or exercise routine. Sudden changes in surfaces, footwear, hill work or returning to exercise too quickly after time off can also trigger shin splints. In the early stage, the pain may settle once you warm up or stop exercising. Later, pain may last throughout exercise and continue afterwards.
As the problem progresses, the pain tends to come on earlier, last longer and interfere with normal training. Mild swelling around the shin may occur, and it may feel tender to the touch. Some people develop shin splints in both legs, while others experience symptoms on one side due to loading differences, foot posture or movement habits. What surprises some is that effective shin splints treatment sometimes may lie in the foot rather than the legs themselves.
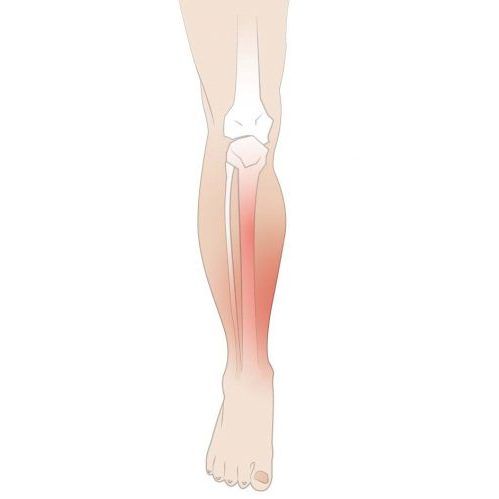
Shin Splints Causes
Shin splints are typically caused by a combination of training load and biomechanics. In simple terms, the lower leg, the muscles, tendons and bone are asked to absorb more force than they are prepared to handle.
The risk is higher for people who are new to running or to an exercise routine, those who suddenly increase mileage or intensity, and athletes who train on hard, uneven surfaces or hilly ground. High-impact sports that involve repeated sprinting and stopping, such as football or basketball, increase the risk. Marching for long periods during NS training can also trigger the same problem, which is why national servicemen in Singapore are a recognised high-risk group.
Foot shape and lower-limb mechanics matter, too. Flat feet, high arches, excessive pronation, tight calf muscles, weak foot and ankle muscles, and poor core and hip control can all increase strain on the shin. Repeated flare-ups may develop into chronic shin splints, especially when people rest just enough for the symptoms to settle, then return to the same loading errors.
To reduce stress on the shin, it is important to address muscles, tendons and bone tissue conditioning and wear the right footwear.

When to See a Podiatrist
You should see a podiatrist if shin splints keep returning, do not improve with simple self-care, or start to affect walking and daily physical activity. Persistent pain and shin pain deserve assessment because not all shin splint symptoms are the same, and you may need tailored support from a foot specialist.
It is particularly important to seek care if you have a small area of very sharp tenderness, mild swelling that seems unusual or flare-ups that recur every time you try to increase your exercise. These patterns can overlap with stress fractures, tendon problems or chronic exertional compartment syndrome, which require different intervention strategies.

How Are Shin Splints Diagnosed?
Shin splints are usually diagnosed through a detailed history and physical examination. A podiatrist will ask when the pain started, what activities bring it on, if there has been a recent change in training, and what footwear you use. The lower leg, ankle and foot are then examined for tenderness, swelling, range of movement and loading response.
At The Foot Practice, diagnosis looks beyond the painful area itself. Tools such as the RehaWalk® pressure-sensor gait analysis treadmill can reveal asymmetrical loading, excessive pronation, inefficient stride mechanics, and other subtle patterns that are hard to see with the naked eye. That matters because shin splint recovery is slower if the underlying mechanical cause is missed.
Imaging is not always needed straight away, but it may be appropriate if the pain is severe, very localised, or not improving as expected. X-rays can help rule out other problems, although early stress fractures do not always show up on plain films. In selected cases, a foot specialist may recommend an MRI or a bone scan if it would affect their care plan.
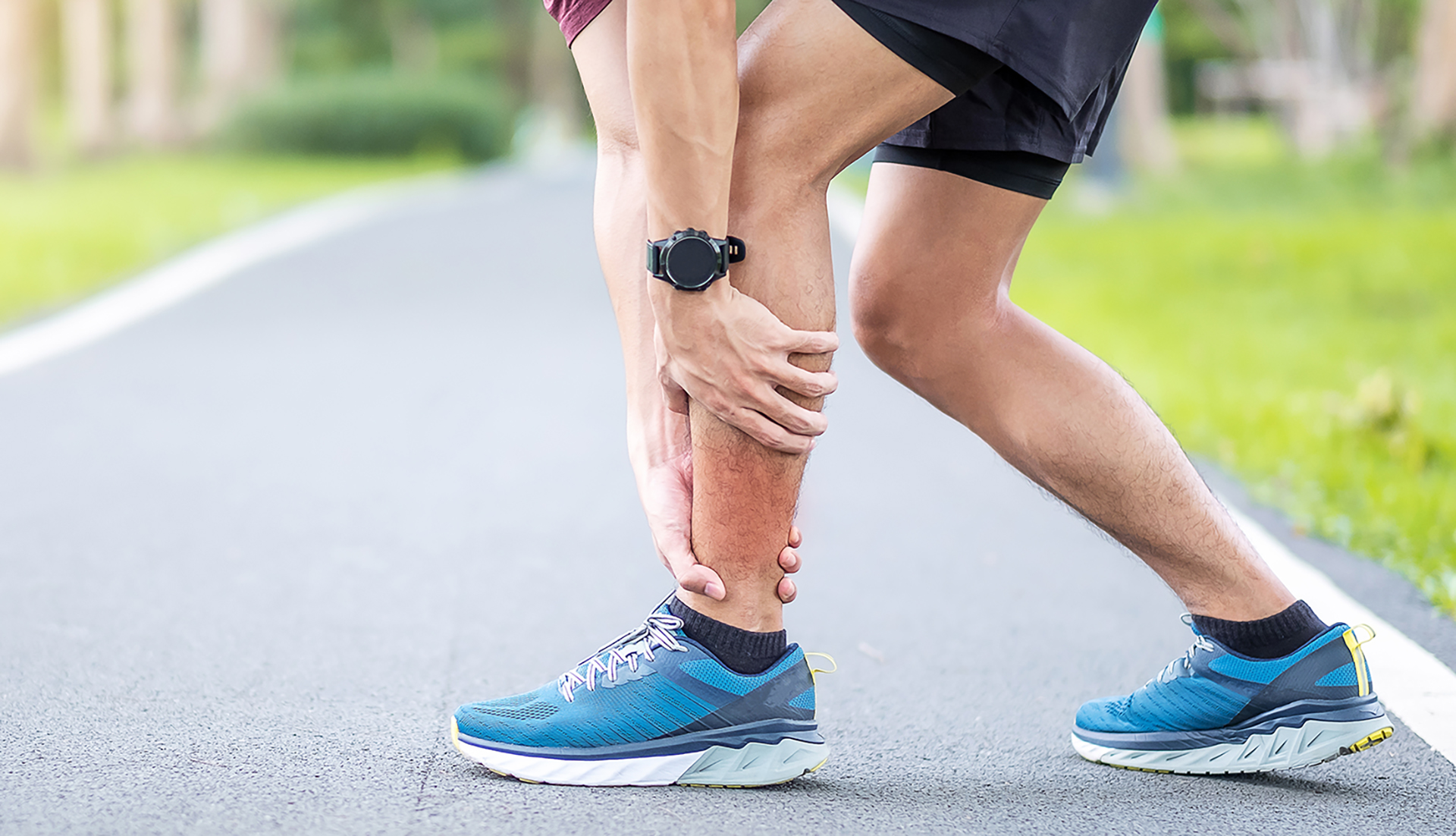
How Podiatry Helps With Shin Splint Recovery
If you are wondering how to heal shin splints, the answer depends on reducing load, settling the irritation, and correcting the root cause.
The first phase usually includes relative rest, ice and a temporary reduction in impact activity. Importantly, relative rest means reducing the aggravating load, not necessarily stopping all movement. Many people can stay active with lower-impact exercise options, such as cross-training, while their shin settles, and the increased blood circulation from the exercise can actually help with the problem. A podiatrist can guide this process to ensure it is safe and sustainable.
Non-Invasive Management
If suitable for the individual, pain relievers such as nonsteroidal anti-inflammatory drugs (NSAIDs) can help in the short term. Gentle calf mobility work, shin splint stretches, stretching exercises, taping and leg stretching may also ease symptoms and reduce stress on the shin. Most shin splints improve within a few weeks with the right approach. The important point is to avoid pushing through pain and returning to full training too quickly.
After that, care becomes more specific depending on the particular case. A podiatrist may prescribe strengthening and mobility exercises for the calf, foot and ankle, as well as exercises that improve balance, shock absorption and lower-limb control. Weakness or stiffness higher up the chain, including at the hips and trunk, may also need attention. Long-term change comes from correcting these biomechanics.
For persistent cases, Shockwave Therapy may be considered as part of a broader care plan. It is not a magic fix, but for most patients, it can support tissue recovery and help resolve stubborn cases. Similarly, Kinesio® tape may give short-term support or symptom relief for some individuals, but it does not replace proper load management, footwear correction or strengthening.
Insoles and Footwear
Footwear and orthotic support can play an important role when biomechanics are part of the problem. Generic shoe inserts may add comfort, but custom arch supports and orthoses provide much more precise control of loading, as well as long-term protection and correction.
For a person with excessive pronation, arch supports can reduce inward collapse and lower the twisting forces transmitted up the tibia. For someone with high arches, the aim may be better shock absorption and even pressure distribution.
This is where a proper footwear review from a podiatrist comes in. Running shoes that are too worn, too soft, too rigid, or unsuited to the person’s foot shape can prolong the problem. Supportive footwear suited to your unique needs can make the difference between shin splint pain and smooth running.
Frequently, patients who struggle with repeated episodes focus only on pain relief and do not address the mechanics underneath. If you are wondering how to heal shin splints properly, footwear, gait and load are often just as important as rest.

How to Prevent Shin Splints
To prevent shin splints, gradually increase your training load, as that is what the body copes best with. Problems arise when training changes faster than bone and soft tissue can adapt.
A sensible prevention plan includes progressive mileage, rest days, calf and foot strengthening, and a warm-up before harder exercise sessions. Hard, sloped and uneven surfaces should be introduced to a training plan gradually rather than all at once. Shoes should be supportive, appropriate for the activity, and replaced before they are badly worn out.
It also helps to vary training. Mixing running with cycling, swimming, strength work, or other lower-impact exercise reduces repetitive stress on the same tissues. Also, listening to early warning signs matters. Shin splint discomfort that starts as a mild nuisance is much easier to manage than discomfort that has become established.