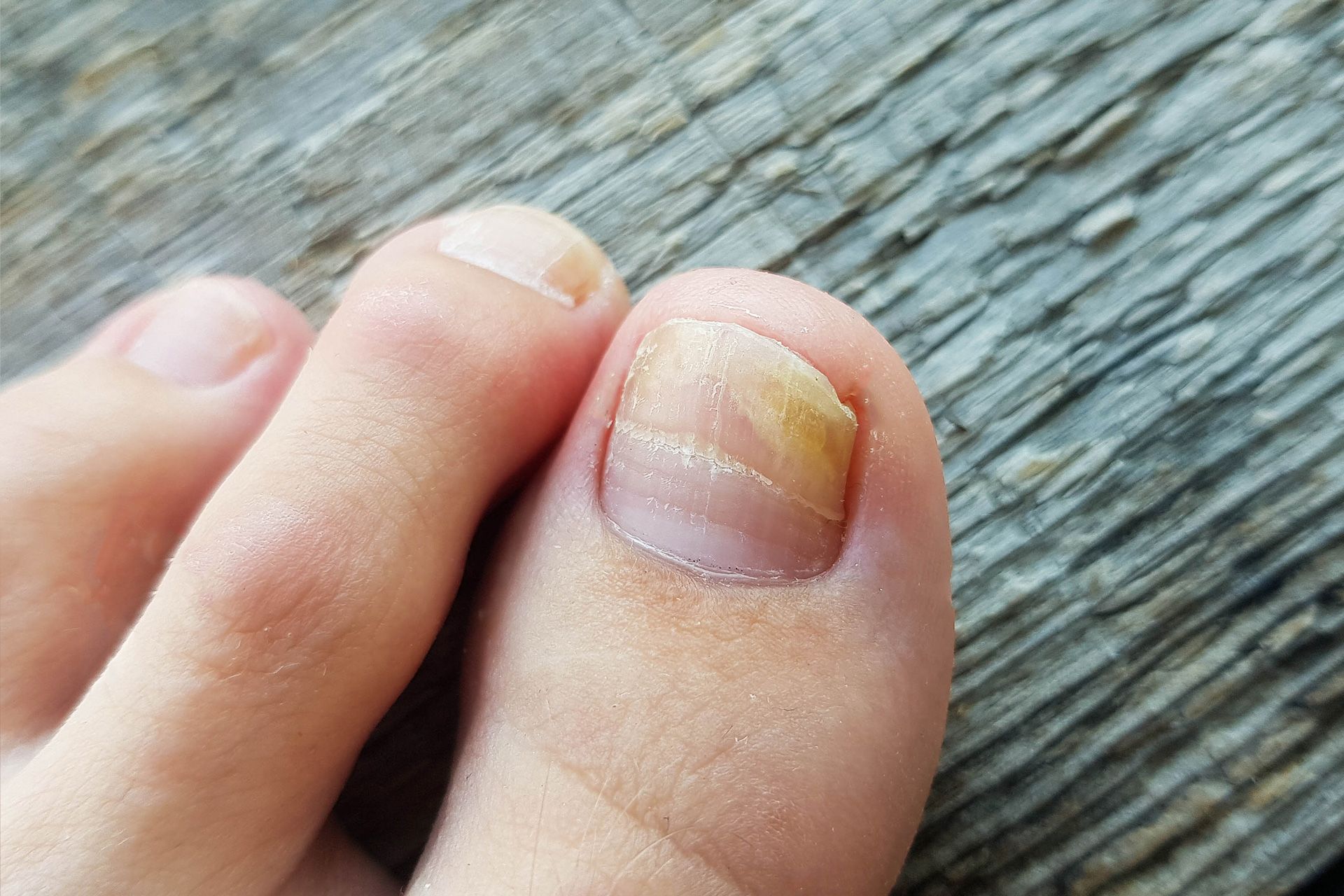
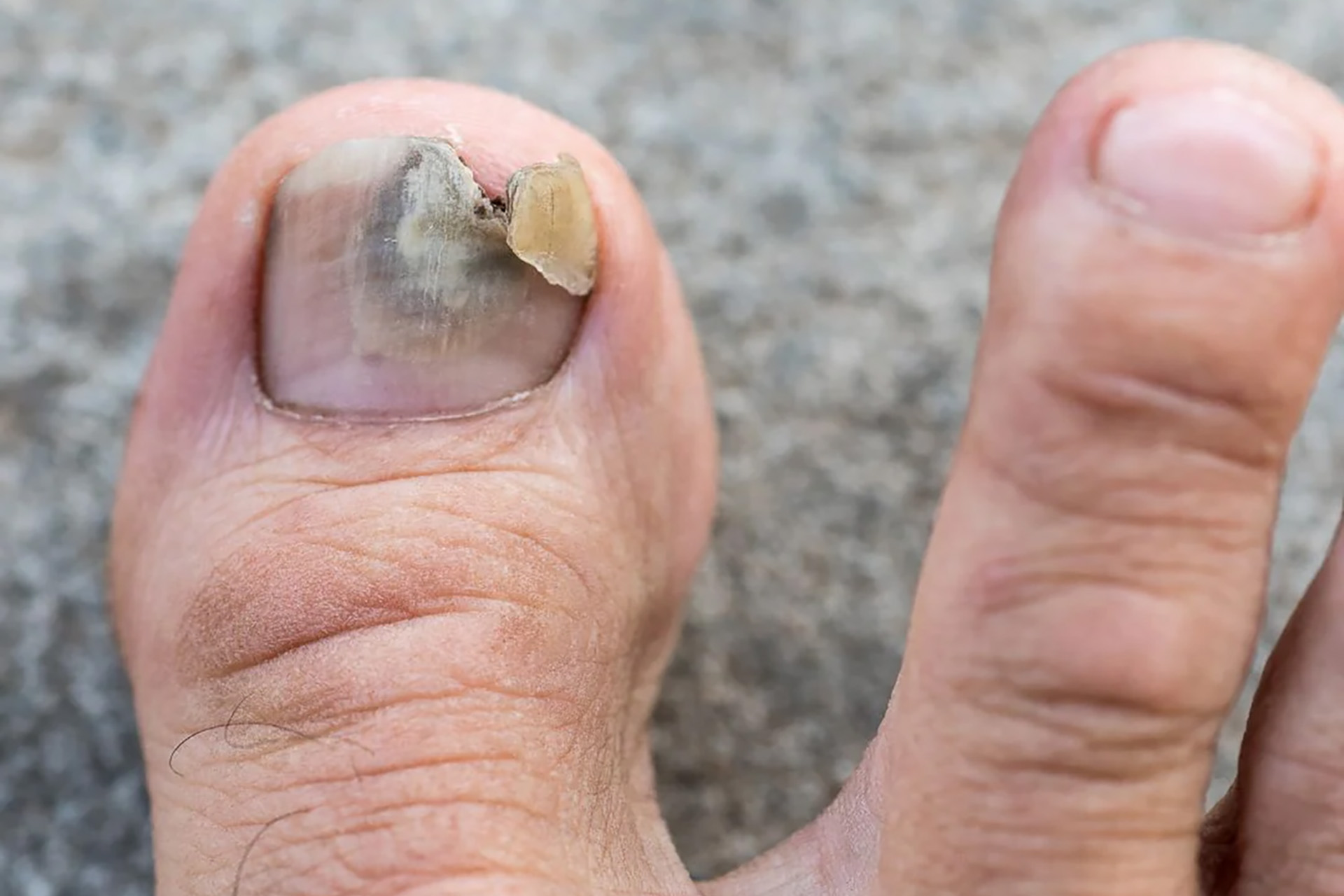
What Is a Fungal Nail Infection?
A fungal nail infection, known medically as onychomycosis or tinea unguium, happens when tiny fungi get into toenails through small cracks, cuts or gaps. Toenail fungus is about ten times more common than fingernail infections because shoes create a constantly warm, moist environment where dermatophyte fungi thrive.
The most common cause is a group of organisms known as dermatophytes, particularly Trichophyton rubrum. Non-dermatophyte moulds and Candida yeasts can also be responsible. A fungal nail infection may also develop after a nail injury or when the same fungi that cause athlete’s foot spread to the toenails.
Once fungus takes hold, it is difficult to clear. The toenails trap organisms beneath, allowing them to grow undisturbed. As toenails grow slowly, clearing a fungal nail infection takes patience and consistent care over many months. Singapore’s year-round humidity and the widespread use of closed-toe footwear make tinea unguium (toenail fungus) one of the most common infection types seen by local podiatrists.
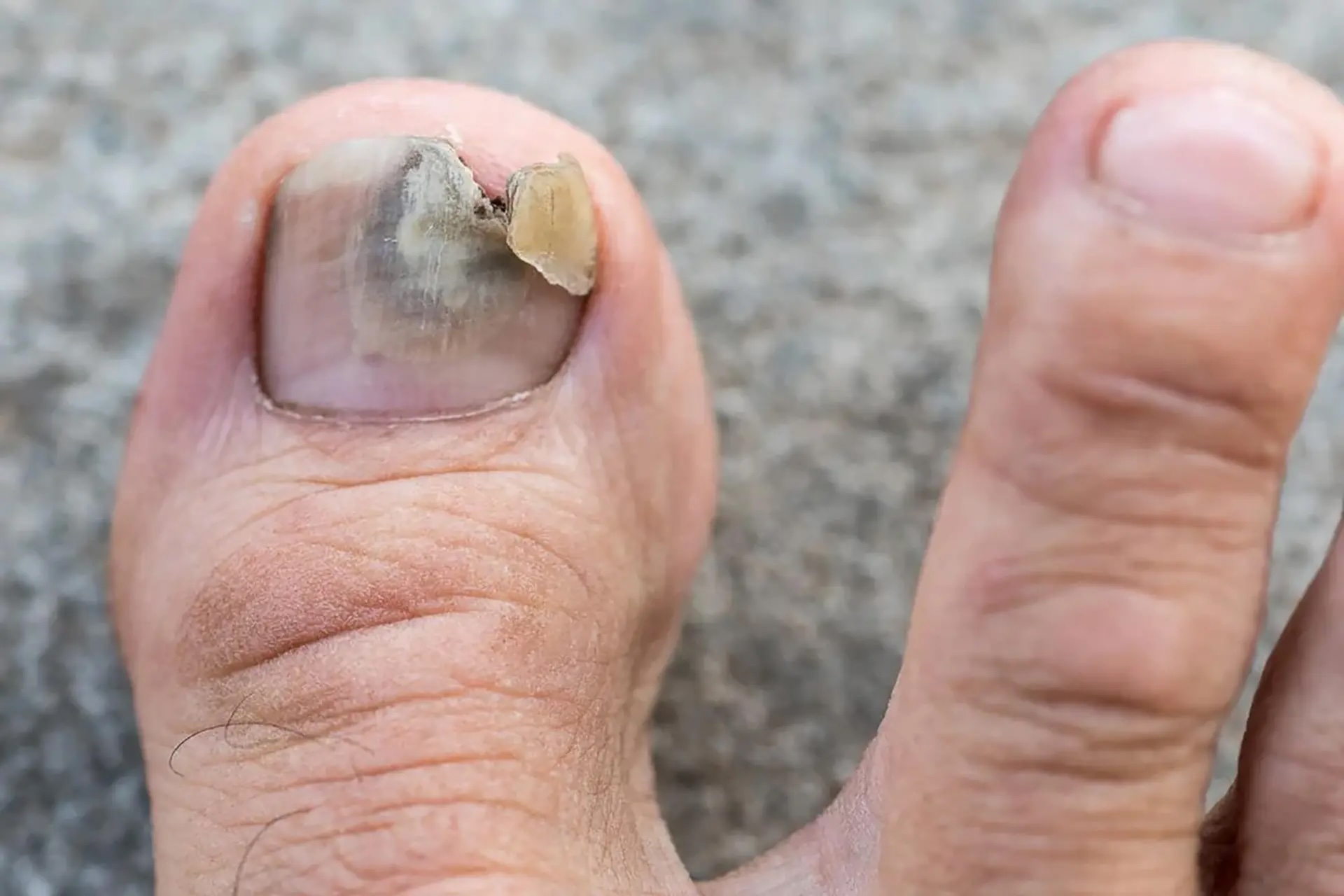
Who Is at Risk?
Certain health conditions and habits raise the likelihood of developing a fungal nail infection. Risk factors for fungal nail infections include:
- A weakened immune system, including those who have had an organ transplant or are undergoing chemotherapy treatment.
- Diabetes, poor blood circulation or peripheral vascular disease.
- Sweaty feet or working in moist environments where your feet get hot and damp.
- Wearing shoes that make your feet hot and cramped, especially those with narrow toes.
- Skin conditions such as psoriasis or eczema that compromise the skin barrier.
- A previous injury or repeated trauma to the toenails. Sharing nail clippers, footwear or walking barefoot in locker rooms and communal showers.
According to the British Association of Dermatologists, toenail fungus affects roughly 10 percent of the general population. Understanding these risk factors can help you prevent fungal nail infections before they start.
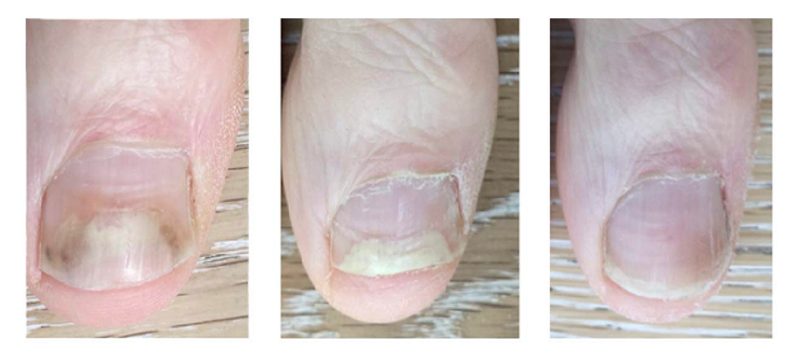
Symptoms
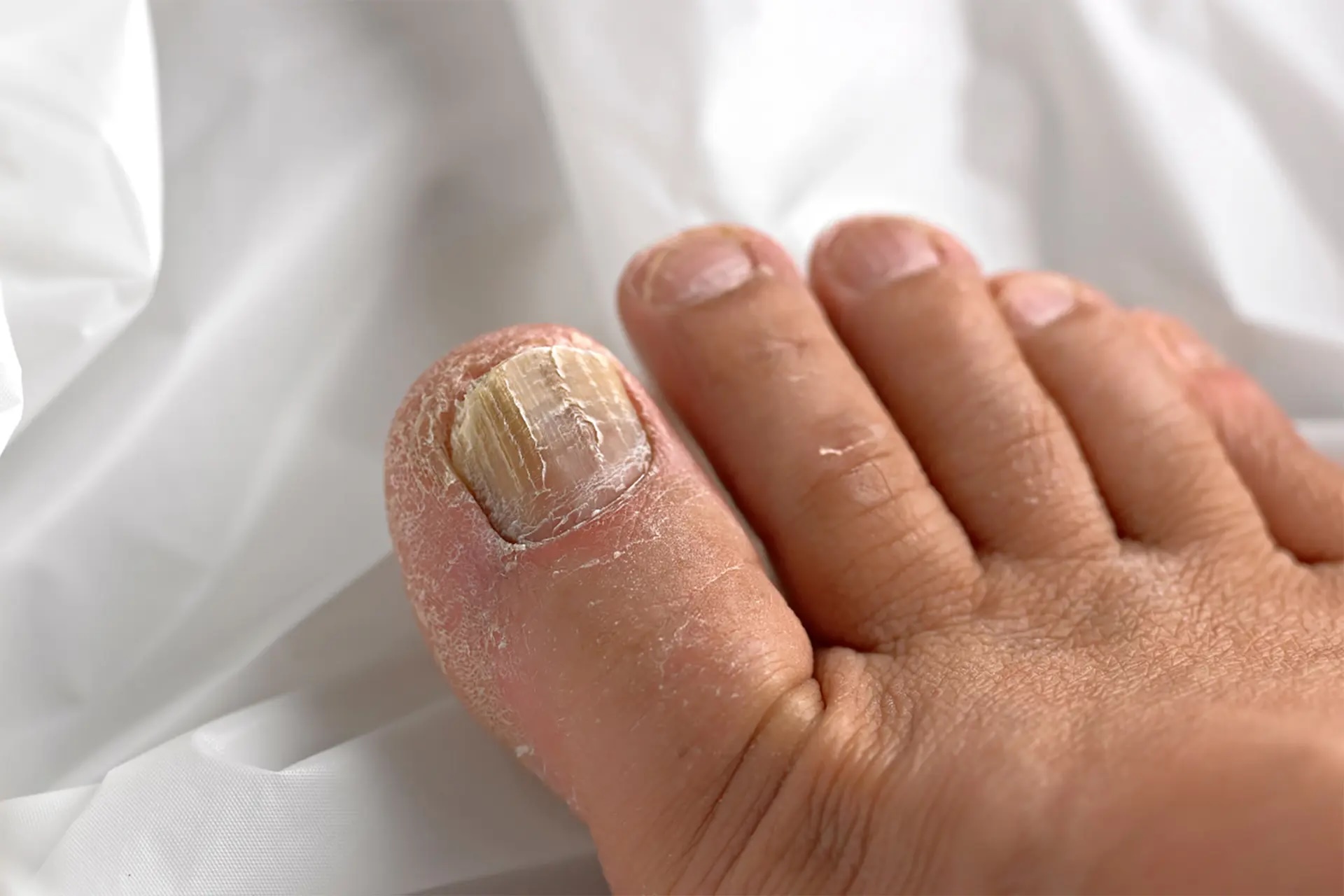
The first sign of a fungal nail infection is usually a white or yellow spot beneath the tip of the toenails. As the infection moves deeper, you may notice:
- Thickening: Toenails become noticeably thicker than normal, resulting in thick nails that are hard to trim.
- Discolouration: Toenails may turn yellow, brown, green or white, a hallmark of fungal nail infection.
- Brittleness: The edges become crumbly or ragged.
- Distorted shape: Toenails may warp or become uneven.
- Lifting: The toenails may separate from the nail bed beneath them, a condition known as onycholysis.
- Odour: Some individuals report a foul odour from the affected nail.
- Discomfort in shoes: Increased thickness can cause pressure and pain, especially in shoes with narrow toes.
Pain is uncommon in early fungal nail infections but may develop as the infection progresses. Most fungal nail infections gradually affect the nail. Left untreated, infected toenails can spread the fungus to other nails and neighbouring toenails, to the surrounding area, a skin condition called athlete’s foot (also known as tinea pedis), or to other people through shared surfaces and tools. Most infections start small but become harder to treat over time.
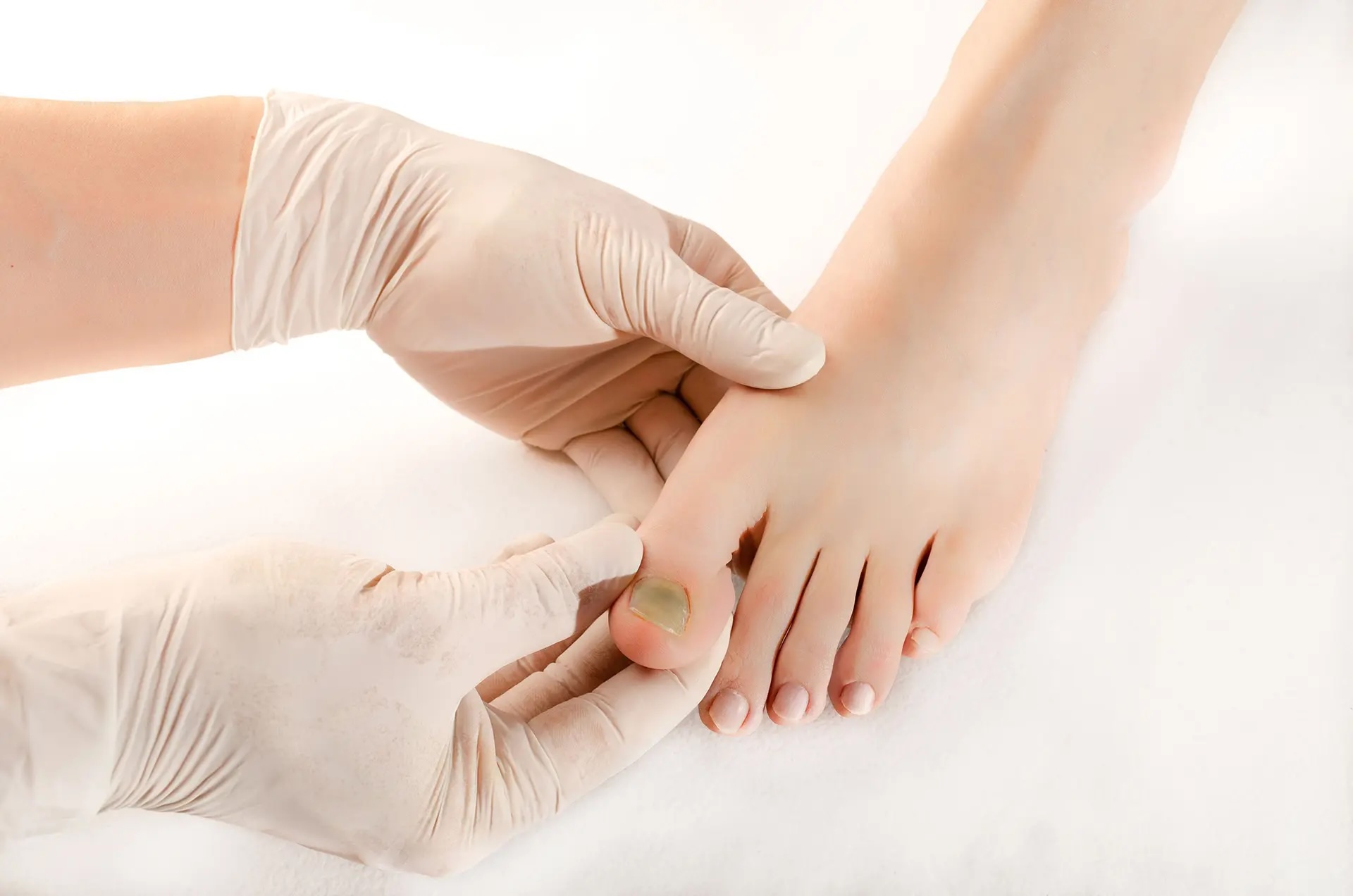
When to See a Podiatrist
See a podiatrist if:
- You notice discolouration or thickening that does not improve with over-the-counter products. Avoid applying nail polish, as it can trap moisture and worsen the fungal infection. The toenails become painful or begin to separate from the underlying tissue.
- You have diabetes, poor blood circulation or a weakened immune system. These conditions slow healing and raise the risk of secondary bacterial infection. The nail bothers you cosmetically or causes foot problems, such as difficulty wearing shoes.
- You have tried home remedies without improvement.
Psoriasis, lichen planus, and trauma can resemble a fungal nail infection and require different management. A podiatrist can tell them apart. Do not apply cosmetic polish to conceal suspicious discolouration; seek professional assessment instead.
Diagnosis
Your podiatrist will examine the colour, thickness, texture and degree of change of the toenails. A small clipping or scraping of debris may be collected and sent for microscopic examination or fungal culture. Tinea unguium (fungal nail infection) can be confirmed through laboratory testing.
This step matters because not all thickened or discoloured toenails are fungal. Identifying the specific fungus helps determine the most appropriate treatment and an effective management plan. Your podiatrist will also assess whether there is an associated skin infection, such as athlete’s foot, since the same fungi often cause both conditions.
Non-Surgical Management
Treatment depends on the severity of your fungal nail infection, the number of toenails affected, and your overall health. Before starting treatment, your podiatrist will outline the available treatment options and create a treatment plan tailored to your situation. It can take months to see results, and repeat infections are common. Here is an overview of the main treatment options.
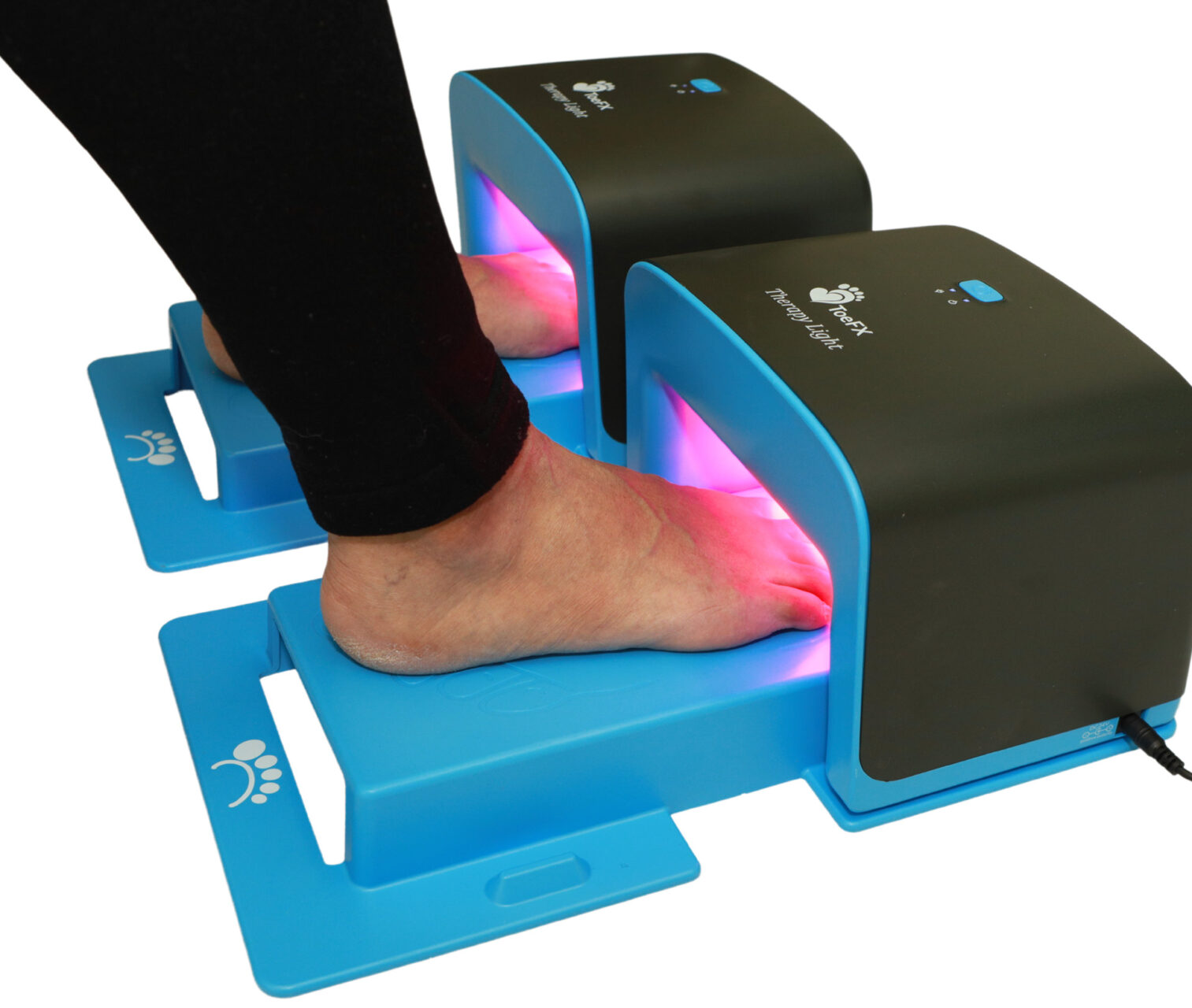
ToeFX Light Therapy
Laser treatment targets the fungus using thermal or photochemical action without oral medication. The therapy may be combined with topical treatments for more stubborn infections. This non-invasive approach uses two wavelengths of light—blue (405 nm) to destroy fungal cells and red (660 nm) to promote blood flow and healing. Each session takes about 20 minutes, including preparation. Most patients need 6 to 10 weekly sessions. Laser treatment does not involve medication, so there are no systemic side effects.
Medical Pedicure (Debridement)
Your podiatrist uses sterile instruments to thin and reduce damaged toenails during a medical pedicure. This relieves pressure, improves comfort in shoes and helps antifungal nail medicine reach the fungal infection more effectively. For severely infected nails, debridement of the entire nail surface may be necessary.

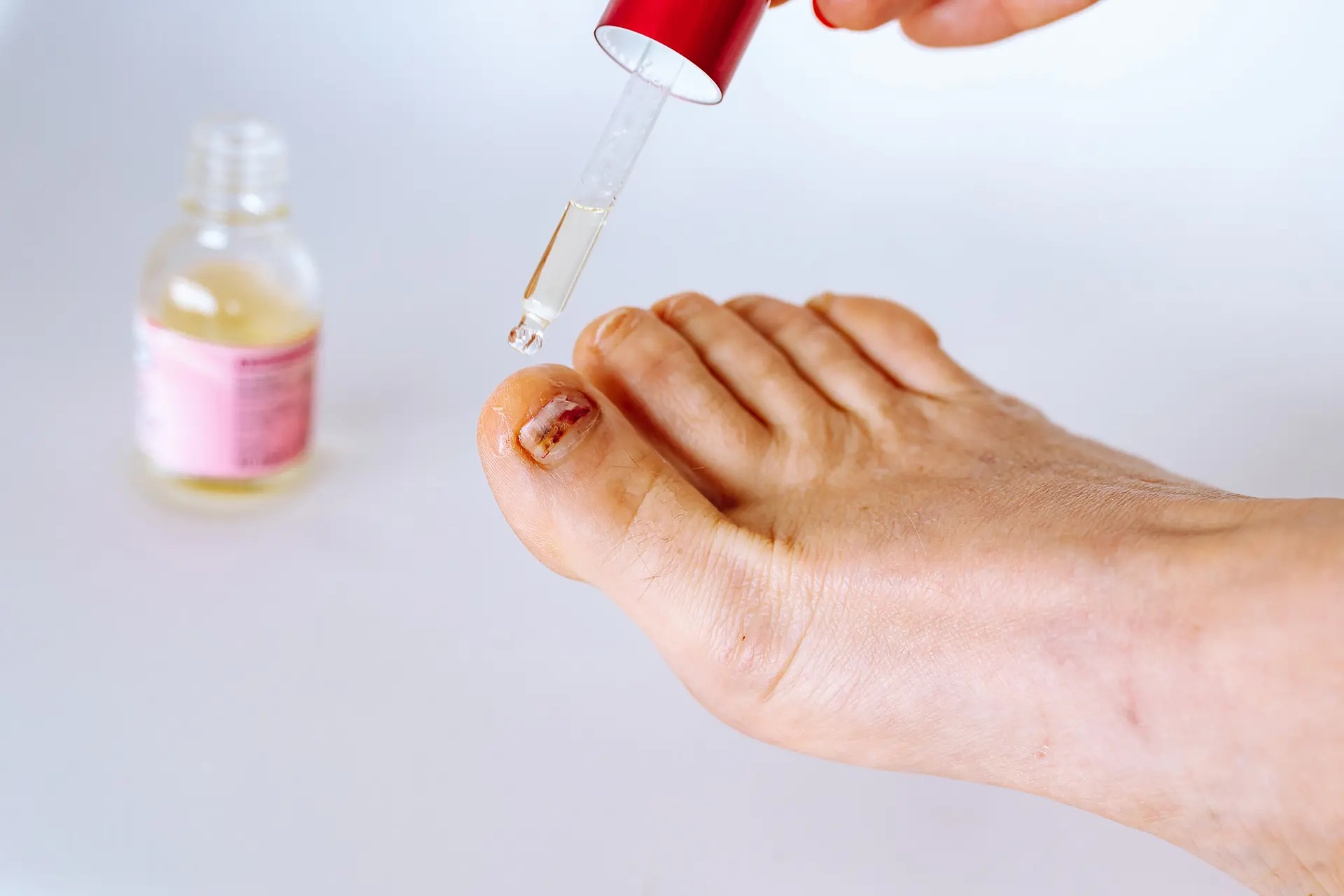
Topical antifungal solutions
For mild fungal nail infections affecting fewer than half of the toenails, your podiatrist may recommend topical treatments such as:
- Antifungal lacquer (amorolfine [Loceryl] or ciclopirox)
- Medicated cream such as Suanfix antifungal cream
You apply the product to the affected nail, typically after filing down the thickened surface to facilitate the topical medication’s penetration. These topical treatments require consistent daily or weekly application for 6 to 12 months or longer. Side effects may include mild irritation. Applying polish to toenails during treatment is not recommended, as it can trap moisture and may worsen the infection.

Antifungal tablets (oral medication)
If the fungal nail infection is moderate to severe, or topical antifungal agents have not worked, your doctor may prescribe antifungal tablets such as terbinafine or itraconazole. These antifungal tablets work by circulating through your bloodstream to reach the fungus beneath your toenails and are usually taken for 3 to 6 months.
Antifungal tablets have higher cure rates than topical medication alone for toenail fungus. As oral antifungal tablets can sometimes cause side effects, including an itchy rash, stomachache, or liver effects, regular blood tests are often recommended. They may not be suitable if you have liver or kidney disease, are undergoing chemotherapy treatment, or take certain other medications. Your doctor will prescribe antifungal tablets only after considering your full medical history.
You will get better results by combining your podiatrist’s care with good home habits. Always keep your feet clean and very dry. Keeping them dry is essential to prevent recurrence. Allow your shoes to air out by rotating pairs and discarding old shoes that harbour fungi. Wear cotton socks that wick away moisture, and use antifungal powder or spray inside your shoes.
Surgical Treatment
If the infection is severe, has spread deeply into the growth area, or has not responded to other fungal nail infection treatment options, your podiatrist may recommend removing part or all of the damaged toenails. Badly infected nails that cause ongoing pain may require this approach. This is a brief procedure performed after the area is anaesthetised.
Removing the entire nail, or part of it, provides direct access for topical antifungal application, improving the likelihood of clearing the fungal infection. A new nail typically regrows over six to twelve months, though regrowth can be slower in older adults or those with reduced circulation.
Nail avulsion is not a first-line treatment. It is reserved for cases in which toenails cause pain, recurrent secondary infection, or significant difficulty with daily activities.
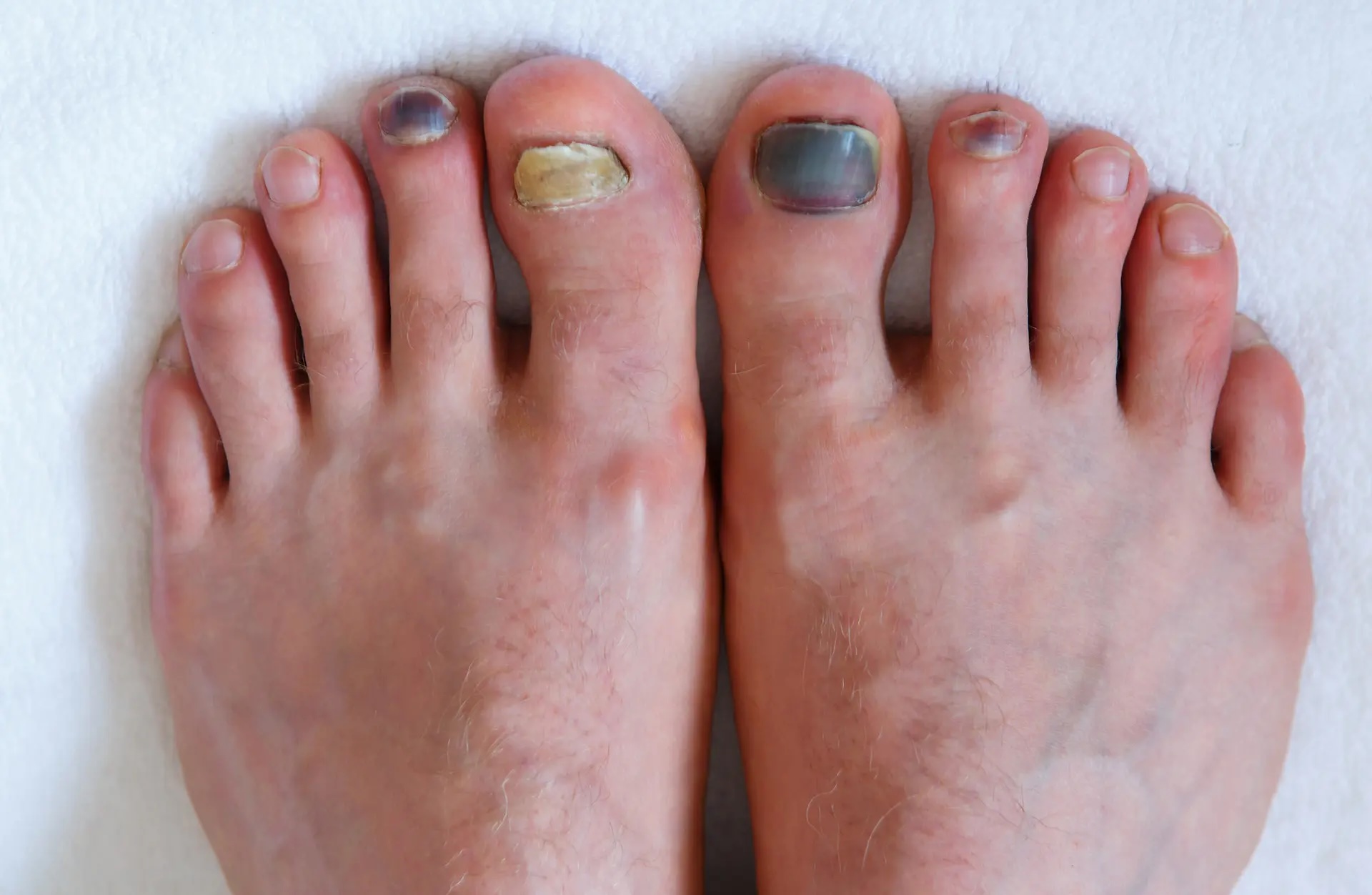
Risks of Leaving a Fungal Nail Infection Untreated
Ignoring a fungal nail infection allows it to get worse over time. The affected toenail can become so thick and distorted that it presses into the surrounding tissue, causing pain and raising the risk of ingrown toenails. The toenail fungus may spread to other toenails or adjacent areas. A common pathway is from one toenail to the next, so early intervention matters.
For people with diabetes, a weakened immune system, or reduced circulation, even a minor fungal infection can create an entry point for bacteria, potentially leading to cellulitis or foot ulceration. If the condition concerns you or you notice it worsening, do not delay. Early professional assessment reduces these risks and shortens the overall timeline.
How to Prevent Fungal Nail Infections
Clearing the fungal infection is only half the job. Preventing recurrence requires consistent daily foot care. You can prevent fungal nail infections with these steps:
- Wear shoes made of breathable materials and discard old shoes that may harbour fungus.
- Wash and dry your feet thoroughly each day, paying close attention to the spaces between your toes.
- Keep toenails short and trim them straight across.
- Avoid cutting them too short.
- Do not share nail clippers.
- Wear breathable, well-fitting shoes.
- Wear cotton socks and alternate pairs so each pair has time to dry.
- Wear flip-flops on a hot day, when appropriate, to let your feet breathe.
- Avoid walking barefoot in communal wet areas such as swimming pools, gym showers, locker rooms and changing rooms.
- Do not share towels, footwear or grooming tools.
- If you visit a salon, consider bringing your own instruments to reduce the risk of cross-contamination.
Treat athlete’s foot promptly. The same dermatophyte fungi that cause infections frequently migrate to the toenails. Tinea unguium often develops following untreated athlete’s foot.
Book a Consultation at The Foot Practice
Whether you have noticed the first signs of a fungal nail infection or have been dealing with a stubborn toenail fungus infection for months, our podiatrists at The Foot Practice on Orchard Road can help. We provide a thorough skin & nail care assessment, accurate diagnosis and a personalised care plan to restore your toenails to health. From toenail and fingernail infections to fungal skin conditions, we provide comprehensive treatment for common toenail fungus and foot problems. Please contact us to schedule a consultation.