Plantar Fasciitis Is a Common Condition of Heel Pain
The plantar fascia, the long fibrous ligament along the bottom of your foot, is one of the body’s strongest structures. It is designed to handle high loads during walking and running. When tiny tears develop in the tissue, they can lead to plantar fasciitis, often described as burning, stabbing, or aching.
Most people with heel discomfort notice it in the morning because the plantar fascia tightens during sleep. As your body warms and you increase movement, the tissue warms up, and the discomfort lessens. However, symptoms may return after prolonged standing, increased physical activity, or prolonged sitting.
Common Plantar Fasciitis Symptoms and Signs
Symptoms of plantar fasciitis typically follow a recognisable pattern: discomfort with first steps, easing as you warm up, then returning after prolonged loading. The key symptoms of plantar fasciitis are first-step pain and tenderness at the bottom of your foot near the heel. Plantar inflammation is also a common symptom. Other signs include:
A flare-up the day following walking or running more than usual can lead to chronic degeneration of the fascia’s fibres. This degeneration also disrupts the pathways for blood flow to the damaged fascia, making it harder for the cells to repair and heal.
- Heel discomfort with the first steps in the morning, or after sitting
- Symptoms after standing for long periods, or after a run or workout
- Tenderness at the bottom of your foot, often closer to the inner side of the heel
- Tight calves or stiffness around the ankle
So, though plantar fasciitis is not necessarily an inflammatory condition, as its name suggests (fasciitis in Latin translates to inflammation), this term is a misnomer, as the condition can occur without inflammation, making plantar fasciosis the more accurate term. However, most people, including ourselves, use the term plantar fasciitis because that is what most mistakenly understand it to be.
What Causes Plantar Fasciitis?
Plantar fasciitis is most often caused by overload, where the load on the plantar fascia exceeds what the tissue can tolerate and adapt to.
Common plantar fasciitis risk factors include:
- Sudden increases in running, walking, standing, or jumping, especially long-distance running
- Tight calf muscles that change how the foot loads, involving calf muscles and lower leg muscles
- Poor shock absorption from worn footwear or hard surfaces
- Foot mechanics, such as prolonged pronation or a very stiff, high-arched foot
- Higher body weight, which can increase strain on the heel bone
- Work and lifestyle patterns that involve long hours on your feet and long periods of standing
Plantar fasciitis in Singapore is often aggravated by prolonged walking, hard indoor flooring, and shoes that look sharp but offer minimal cushioning or arch support. Supportive shoes with good arch support can help reduce stress on the plantar fascia, especially if you often wear flat shoes or flip flops.
Is It Always Plantar Fasciitis?
In many cases, diagnosing heel discomfort as plantar fasciitis is incorrect, as numerous muscles, soft tissues and nerves interact with the heel. A key goal of assessment is to confirm that the symptoms are consistent with plantar fasciitis heel pain and to rule out other causes.
Though plantar fasciitis is not necessarily an inflammatory condition (fasciitis in Latin translates to ‘inflammation’). The term is a misnomer, as the condition can occur without inflammation, making plantar fasciosis the more accurate term. In many people, plantar fasciitis is limited to inflammation, but it can still involve inflammation early on and during flare-ups. However, most, including podiatrists like us, use the term ‘plantar fasciitis’ because that is what most mistakenly think it is.
Other conditions that can mimic plantar fasciitis include:
- Heel fat pad irritation (often more central under the heel)
- Nerve-related heel discomfort (may include tingling, burning or symptoms that spread)
- Stress injury to the heel bone, including a stress fracture
- Irritation around nearby tendons and soft tissues
- Inflammatory joint conditions (especially if multiple joints are involved)
- Heel spurs and bone spurs can be present even when they are not the main driver of symptoms
This matters because the best management plan depends on an accurate diagnosis and the exact location of the plantar fasciitis pain. If you feel pain only in one foot or if symptoms are sharply localised, it is sensible to get assessed by a medical professional.
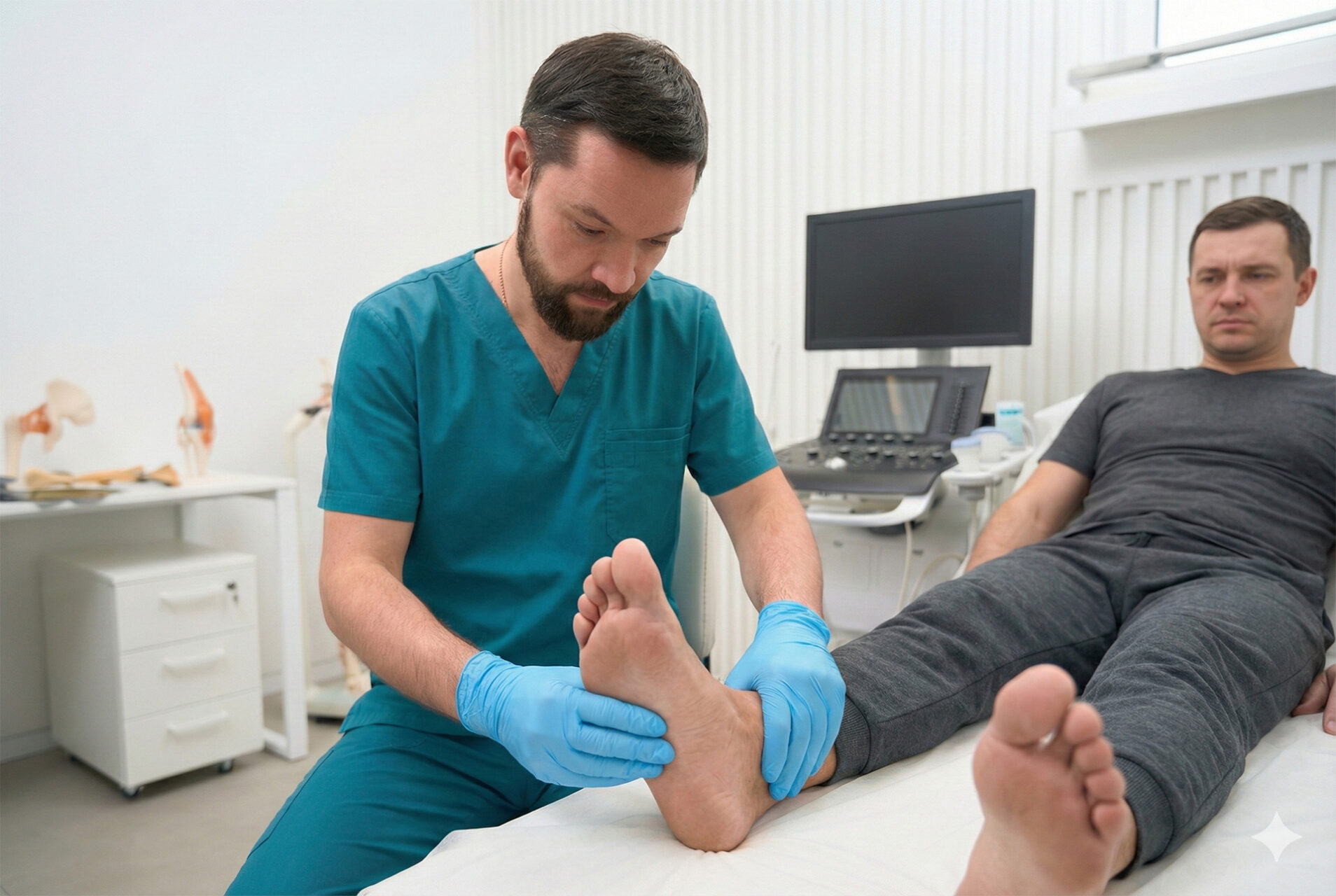
How Is Plantar Fasciitis Diagnosed?
Plantar fasciitis is diagnosed based on your medical history and a physical examination, with the location and pattern of symptoms guiding the diagnosis.
A podiatrist may assess:
- Where the heel is most tender, and what movements reproduce symptoms
- Foot posture and how your arch behaves during standing and walking
- Calf tightness and ankle flexibility
- Big toe mobility and how efficiently the foot ‘locks’ during push-off
- Footwear wear patterns, load points, and whether you walk barefoot at home on hard floors
Imaging tests such as X-rays, ultrasounds, or MRI scans may be considered when symptoms persist, are severe or atypical, or are not improving as expected, or when another diagnosis needs to be ruled out.
Can A Podiatrist Help With Plantar Fasciitis?
A trained podiatrist with experience managing sports injuries and foot and ankle conditions can assess your heel and develop an appropriate management plan for plantar fasciitis. Plantar fasciitis treated early is often easier to settle because the foot has not adapted to protective movement patterns.
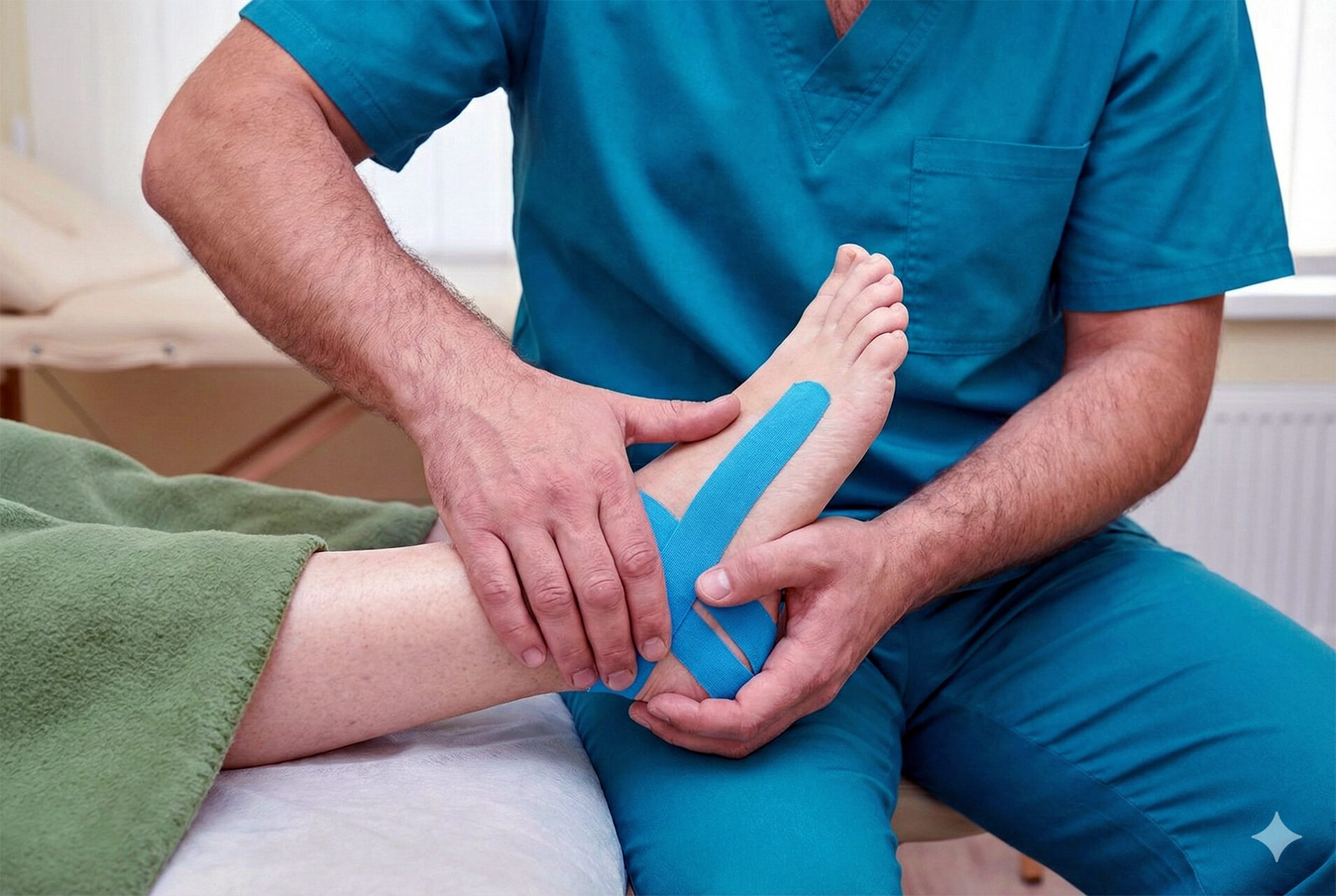
The most immediate step to address plantar fasciitis is to reduce the forces that are stressing the plantar fascia. One offloading technique is low-dye strapping, in which your specialist applies medical tape to the foot to support the affected areas, such as the arch or ankle. This can be very helpful either before or during a running event.
However, taping is only a short-term solution that addresses immediate discomfort and irritation. An experienced podiatrist can offer a range of non-invasive intervention strategies to help with plantar fasciitis, addressing the root cause with advanced modalities and careful assessments.
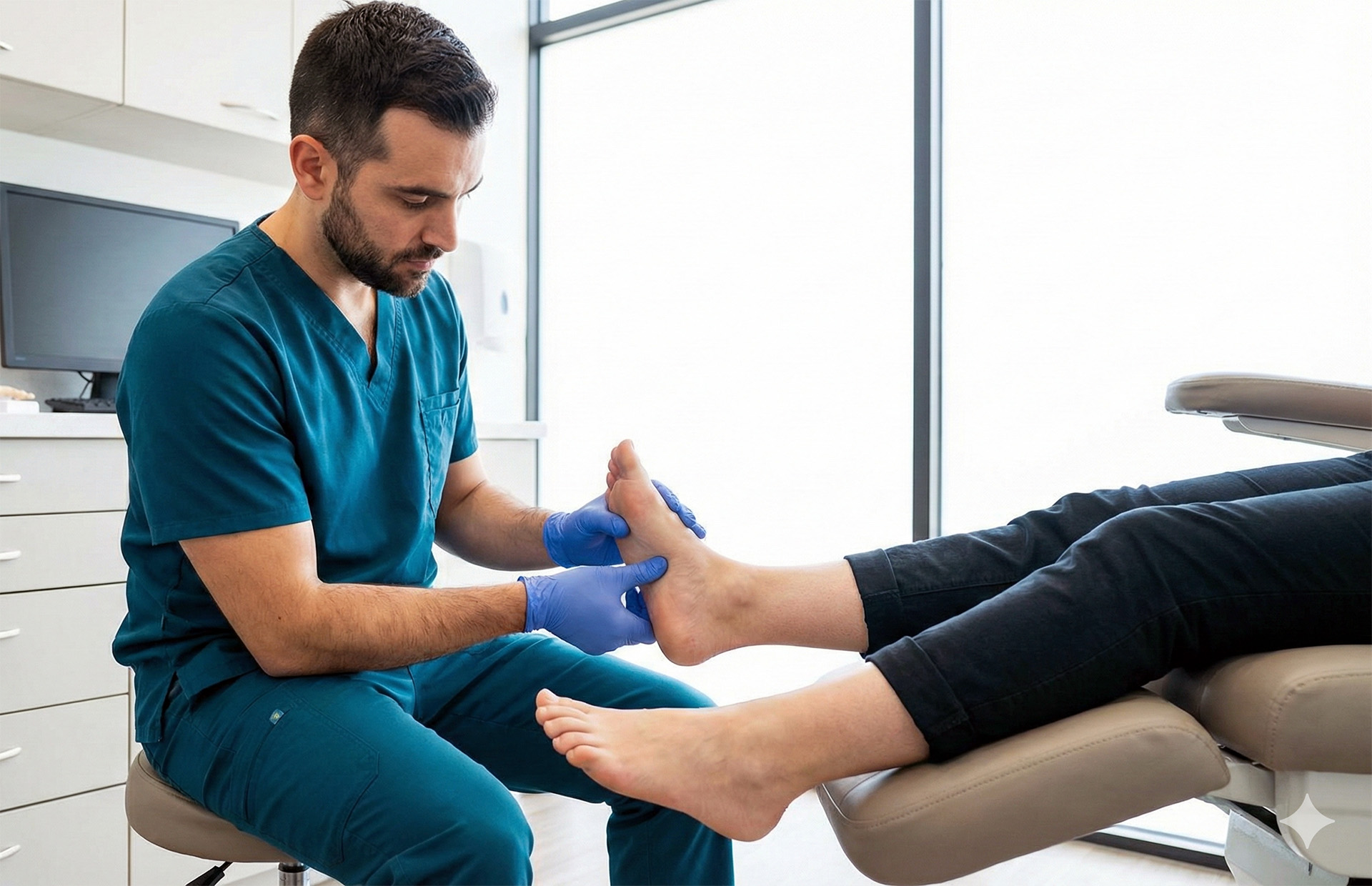
Non-Surgical Management for Plantar Fasciitis
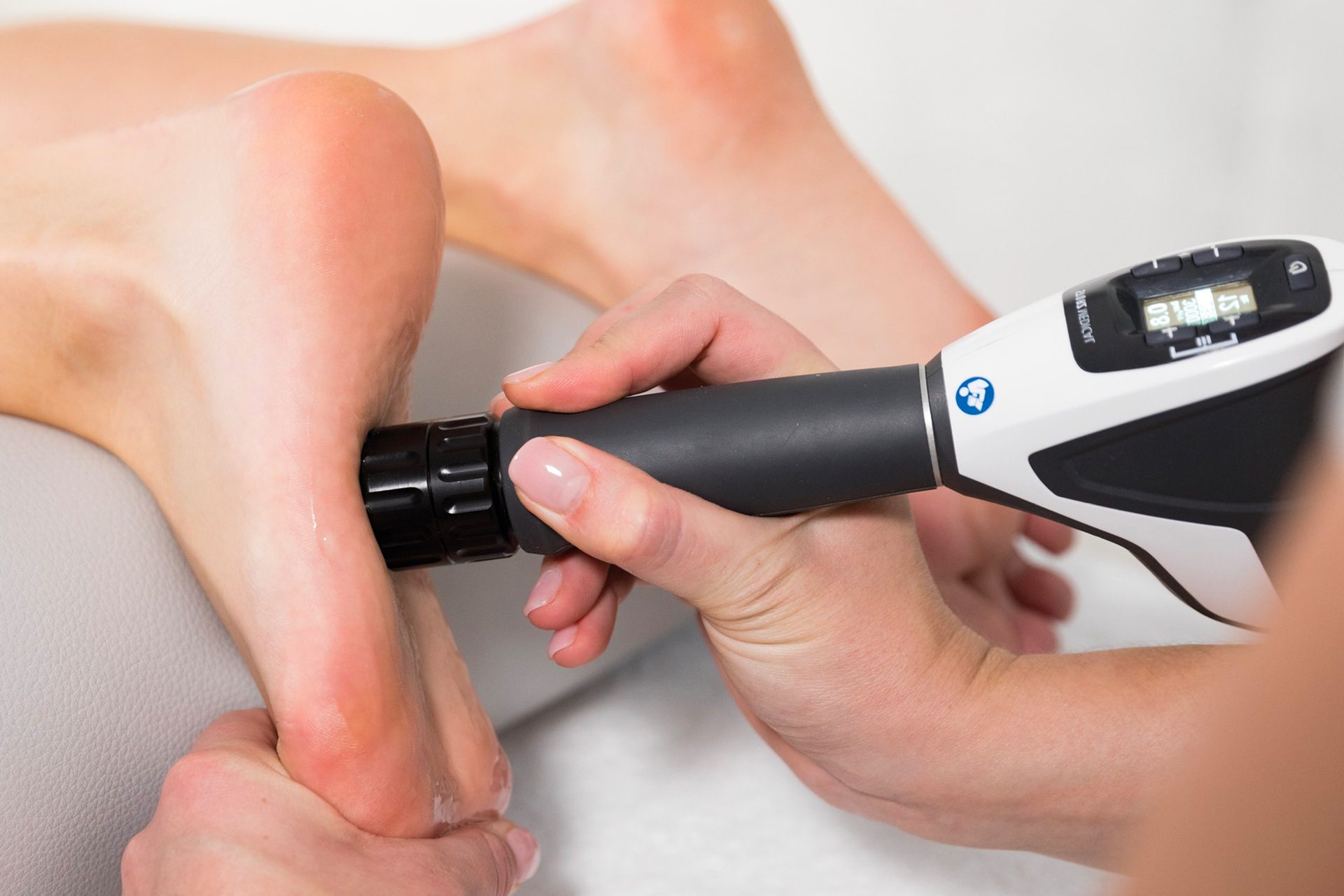
Shockwave Therapy
Shockwave Therapy for plantar fasciitis can be part of a balanced care protocol, especially when symptoms persist. Extracorporeal Shockwave Therapy uses sound waves to support the healing response and can increase blood flow to the affected tissue as part of a broader treatment plan. Shockwave Therapy may also be considered an alternative treatment for selected cases of plantar fasciitis, in addition to other care.
Footwear Assessment
Tight calf muscles are a risk factor for overcompensation, which can contribute to plantar fasciitis. An assessment with our podiatrist can help you identify footwear with the right balance of cushioning, stability, and support. In some cases, a higher heel-to-toe drop may initially reduce strain as symptoms settle.
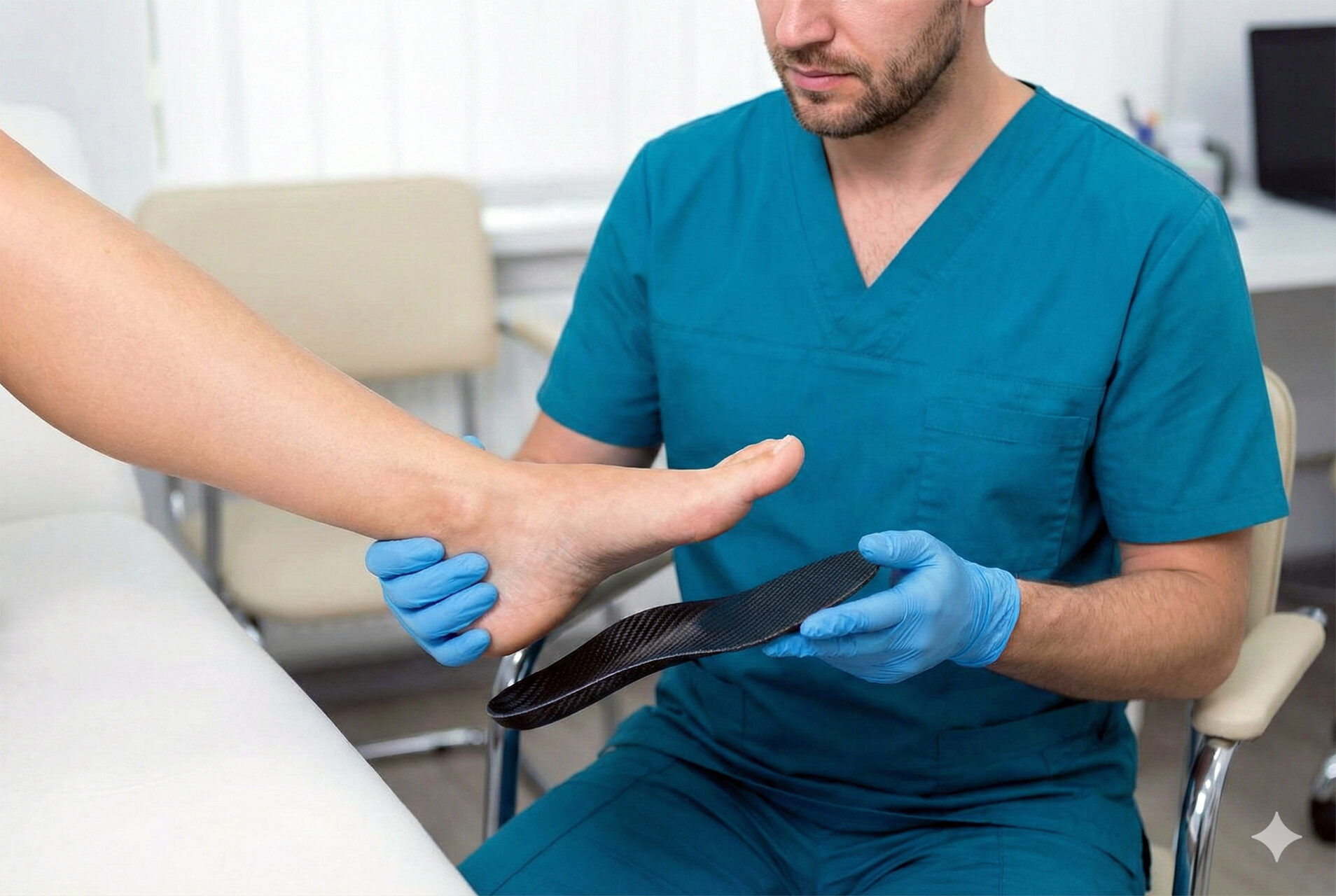
Orthotic Insoles
Orthotic plantar fasciitis insoles can help correct extreme foot pronation, in which the foot’s arch flattens due to the angle of the step. In many cases, foot orthotics reduce symptoms by altering foot strike, thereby reducing the excess force transmitted through the plantar fascia. Custom-made or premade orthotic insoles can be catered to your gait to help the plantar fascia function properly.
Exercises and Mobilisation
Regular stretching throughout the day can help build strength and flexibility in the plantar fascia and Achilles tendon. Your podiatrist may recommend using a cooled rolling instrument under the foot to help manage discomfort, such as a frozen water bottle. These plantar fasciitis stretches and exercises can form part of a foot mobilisation and strengthening plan designed to improve foot loading.
Night Splints
As mentioned, one problem with plantar fasciitis is that the foot muscles can tighten overnight, worsening symptoms in the morning. Night splints help stretch the foot overnight and reduce first-step pain for some people.
Other Plantar Fasciitis Treatments
Other treatments for plantar fasciitis include steroid injections, a short-term walking boot for persistent cases, and physical therapy focused on calf stretching and progressive loading. If symptoms persist, surgery, such as plantar fascia release or gastrocnemius recession/release, may be discussed.
Simple, Practical Steps You Can Do Now
The goal is to relieve heel pain while keeping you moving safely and reducing plantar fasciitis heel pain without triggering a flare-up
- Reduce painful load for a short window: cut hills, speedwork, long walks and hard-surface runs
- Swap in low-impact cardio temporarily: cycling, swimming, rowing, or upper-body conditioning
- Wear supportive shoes at home rather than going barefoot on hard floors
- Keep stretching consistently: calf and plantar fascia stretching, but avoid pushing into sharp symptoms
- Avoid sudden footwear changes during a flare-up, especially to minimalist shoes with little support
If your heel discomfort is severe, keeps worsening, or becomes very focal, it is sensible to get it assessed rather than pushing through.
Can Plantar Fasciitis Cause Toe Pain?
The cause of plantar fasciitis remains incompletely understood, as clinical research continues to evaluate the condition to deepen our understanding. From our experience with patients who come into our podiatry clinic, the factors that contribute to heel symptoms include:
- Overuse injuries that began as a niggling nuisance before becoming a debilitating issue
- Heel spurs and ankle instability
- Lack of big toe mobility
Most foot stability comes directly from the big toe and the arch of the foot. When the foot strikes the ground, the arch and big toe help evenly distribute impact forces across the foot. A healthy gait relies on the ability of the big toe to have a greater toe upward bend at about 50 to 90° when the body’s weight passes over the foot. When big toe mobility is restricted, the foot may compensate and overload the plantar structures, which can make symptoms feel as if they spread into the arch or forefoot.

Can Plantar Fasciitis Go Away on Its Own?
Plantar fasciitis can resolve on its own, but symptoms may take months to subside, especially if the factors driving the overload are not addressed. Further complications and injuries to other parts of the body can occur without proper diagnosis and care.
Each person’s biomechanics differ, and an appointment with our podiatry team at The Foot Practice can help you understand the root causes of the movement patterns that contribute to your plantar fasciitis and reduce the likelihood of recurrence.
How Can I Prevent Plantar Fasciitis?
Following an initial assessment, your podiatrist will develop a tailored care plan and discuss a management plan for plantar fasciitis that aligns with your goals. The next step in ‘curing’ plantar fasciitis is to progressively increase activity levels.
For example, it may be safe to run with plantar fasciitis contingent on the plantar fascia gradually adapting until it can withstand the usual running pressures. If you are searching for how to get rid of plantar fasciitis or how to heal it quickly, the safest approach is a structured plan that first settles symptoms, then carefully and steadily rebuilds capacity.
You can also ease recovery by wearing podiatrist-prescribed arch supports or shoe insoles as you return to your preferred running level. Ultimately, our goal at The Foot Practice is to minimise the risk factors for plantar fasciitis, so your foot is ready for proper weight-bearing activities and can recover optimally.
Through our pioneering 3D infrared analysis, our team develops a gait retraining programme to help you avoid future injuries. The technology examines aspects of your gait, including foot pronation, hip extension and abduction, dorsiflexion, maximum eversion, and other factors, to re-educate your gait and improve running efficiency while reducing injury risk. Using real, measurable data, we monitor your progress to support proper foot function and address your plantar fasciitis.
When Should You Seek Assessment?
Book an assessment soon if:
- Heel discomfort persists beyond 2 to 3 weeks despite load changes
- Symptoms are getting worse rather than gradually improving
- Symptoms are very focal in one spot, or you suspect a stress fracture
- You have numbness, tingling, or burning that suggests nerve involvement
- You have diabetes or circulation concerns, and any new foot symptoms
FAQs about Plantar Fasciitis
How do you relieve plantar fasciitis pain?
Should I stretch my plantar fascia or rest it?
Is walking good for plantar fasciitis?
What is the best exercise for plantar fasciitis?
Do I need orthotics for plantar fasciitis?
The Foot Practice Can Help
If you are experiencing plantar fasciitis, contact our podiatry clinic before it becomes a chronic condition or a more complex injury.
The Foot Practice’s integrative approach includes footwear analysis, biomechanics training, orthotic care, and other interventions customised for your needs. If you are seeking plantar fasciitis treatment in Singapore, we provide a clear plan, including treatment and return-to-activity guidance, based on your assessment. Contact The Foot Practice today to schedule an initial consultation with our experienced sports podiatrist in Singapore.